Do carb burners live longer?
I've been looking at respiratory quotient a bit after my post series on the Ranneries paper on metabolisms of the formerly obese (Part I, Part II, Part III) and found some interesting things. One is this paper:
Resting Metabolic Rate and Respiratory Quotient in Human Longevity
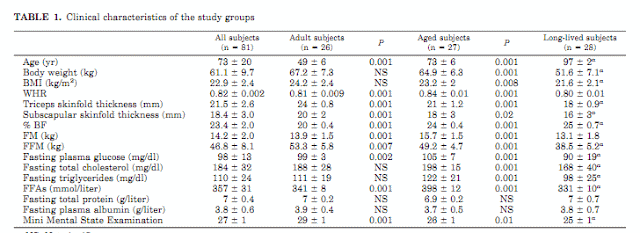
In this study they compared three groups of women, I've included the table of various parameters below:
The groups were relatively large (almost 30 participants per). The "adults" averaged almost 50 years old with the aged being roughly 25 years older (73) and the long-lived almost twice the age of the adults (97). My point in repeating that information is that while their adults were already middle aged (and as women likely dealing with some issues related to menopause), the other groups were significantly older.
All subjects consumed a standard diet for two weeks prior to assessments consisting of 50% carbs, 27% fat and 23% protein. I would note this is a bit higher in protein than usual (and perhaps lower in fat). The metabolic data is shown below:
RMR = Resting Metabolic Rate FFM = Fat Free (aka Lean) Mass WHR = Waist-to-Hip Ratio
Despite the fact that in the whole group of subjects an age-related decline in RMR and Rq was found, the analysis restrained to long-lived subjects showed in this group RMR and Rq greater than that found in aged subjects. Such a difference might be explained by the changes in anthropometrics features because long-lived subjects had lower BMI, FFM, and WHR than aged subjects. Our results suggest that long-lived subjects are less prone to the metabolic derangement*, normally occurring with age. To this regard, previous studies on human longevity have underlined the role of various metabolic, endocrine, and biological factors as potential determinants of a successful ageing. *It's official! A scientist used the term ;-)
As a reminder, a higher respiratory quotient, Rq or RQ, is indicative of oxidizing a higher proportion of carbohydrate for energy vs. fat. I also point out that, as in the Ranneries study, metabolic rate and VO2max are correlated.
Now, a known consequence of aging is insulin resistance. So I did a little looking into how IR might impact one's RQ. This is by no means an exhaustive search, but just a couple of cites:
... free fatty acids induce insulin resistance in humans by initial inhibition of glucose transport/phosphorylation which is then followed by an ~50% reduction in both the rate of muscle glycogen synthesis and glucose oxidation.
This would mean IR would decrease RQ.
Basal rates of glucose production were similar in the young and elderly participants and were suppressed completely in both groups during the hyperinsulinemic-euglycemic clamp. In contrast, the rates of glucose infusion required to maintain euglycemia during the clamp and insulin-stimulated rates of peripheral glucose uptake were ∼40% lower in the elderly participants. Basal energy expenditure and respiratory quotient both tended to be lower in the elderly participants.
The IMCL [intramyocellular lipid - aka fat in muscle cells] content in the soleus muscle was increased by ∼45% in the elderly participants as compared with controls. Intrahepatic triglyceride content was also increased by 225% in the elderly participants as compared with controls ...
Because increases in intramyocellular and intrahepatic triglyceride content could occur secondarily to increased fatty acid delivery from lipolysis, we also examined this process in vivo. ... Basal rates of whole-body glycerol turnover and insulin suppression of glycerol turnover during the clamp were similar in the elderly and control participants. Consistent with this finding, the interstitial glycerol concentrations, assessed by microdialysis, decreased by a similar degree during the clamp in both groups. Taken together, these data suggest that insulin resistance was confined mostly to skeletal muscle and that increased basal rates of peripheral lipolysis, and/or defects in insulin suppression of lipolysis, do not play a major role in causing the increased intramyocellular and intrahepatic triglyceride content in the elderly
This study seems to imply that mitochondrial dysfunction is in the handling of carbohydrates as primary substrate rather than of fatty acid utilization. The IR associated with aging was of a peripheral nature at the utilization end. This is in contrast to what we see in obesity. Unlike what we saw in the formerly obese study, the reduced resting energy expenditure of the elderly v. adults and long-lived is accompanied by a reduction in glucose oxidation, not fat oxidation. The implication for the FO study was that reduced lipid oxidation at rest was responsible for the lower energy expenditure and thus likelihood of regain, etc. In this study (also in just women), the reduction in energy expenditure that accompanied aging was concurrent with a reduction in carbohydrate utilization.
... as well as being the predominant postprandial anabolic hormone for substrate utilization, insulin is also a major regulating factor of mitochondrial oxidative phosphorylation in human skeletal muscle.
That paper contains the nice graphic at right.
It is a reasonable interpretation, then, that the reduced RQ of the aged vs. the adults and long-lived is an indication of insulin resistance, and the concomitant reduction in RMR vs. the others can be attributed to reduced stimulation of oxidative phosphorylation by insulin.
Now ... notice the *?* in the post title here ... this is because there's quite a bit of speculation in this post, and cause/effect is never clear in such studies. If one adopts a diet favoring burning carbs for energy will they live longer given their genetic makeup ... or vice versa? Or is it that there are genetically gifted folks who live longer? If the latter, it would seem that insulin sensitivity and good carb burning ability is, indeed, a "gift". One thing that we can say with a degree of certainty is that a higher RQ in conjunction with faster burning of fuel does not seem to have hurt these 28 long-lived ladies. The glucose burning vs. fat burning did not produce more ROS or whatever is attributed to deterioration with age. Indeed since they are still live and kicking, one could conclude perhaps the opposite was the case. The other thing that seems rather clear is that the long-lived retained their insulin sensitivity at the muscle cell level. Not quite comparable to those half their age, but rather impressive compared to those 25 years younger experiencing declines.
This is yet another study that demonstrates the importance of maintaining insulin sensitivity. In particular it shows that skeletal muscles seem to like to run on some glucose too. It's not just for the brain. If it were not a good fuel for muscles to run on, and fats preferred, I think we would find a lower RQ amongst the long-lived. If running on glucose were wasteful, metabolically "dirty", sub-optimal ... why do the declining aged burn less of it while the long-lived still happily burn it? There's this catchphrase of "metabolic flexibility" floating around the net these days where folks seem to be worried over losing their fat-burning abilities. I would say this study offers food for thought over which substrate is more critical to worry over maintaining the metabolic machinery to handle.

Comments
And call me a cockeyed optimist, but I think it's plausible that one might actually recover from metabolic "derangement," not treat it as an irreversible condition.
You are a cockeyed optimist. But I think it's plausible too.
On the second chart, the most striking thing for me is how different the results were for the "aged" as compared to both the adults and the long lived. TV goes from .47 to .35 for the aged, to .43 for the longlived. VO2 goes from 232 to 170 and then back up to 216. One possibility is that the sample sizes are just not big enough, and the "aged" group is an anomaly. Or I suppose it's also possible that the aged group includes a bunch of women with bad numbers, that those numbers deteriorate a whole lot from "adult" classification to "aged", and that the ones who experience this deterioration will die before they get to "long lived" classification.
I know you say that the sample groups were "relatively large". It looks to me like this is basically a population study, and three groups of thirty people doesn't strike me as being large at all.
@Duffy: When they looked at all subjects, they saw RQ, REE and such decline with age statistically. But when they broke it out to three age ranges, they saw what they saw. I suppose it could be an anomaly, but statistically speaking those sample sizes argue against that. The authors acknowledge the limitations of the cross-sectional study. What they postulate is that with age, metabolism does decline, but those for whom it does not, or to a lesser extent, survive longer -- thus are "weeded out" in the >95 yo group. No one study is going to hold all the answers. If I come across one that measures REE and RQ prospectively for decades I'll be sure to share it!
Yep.
I would love to see a study comparing 10 year VLC'ers to others age/weight matched, preferably with some attention to "dietary adherence" to what each group considered "healthy".
The more I read the less I think very low carb is advisable as a "lifestyle". It seems more useful for weight loss but I'd predict long term VLC'ers have rather slowed metabolisms
it's simply not so. I have been relatively low-carb since 2003. I was very low carb between 2007 and earlier this year (when I started eating more of Paul's 'safe starches' because of issues with mucous and joint problems). I weigh 53 kg and my metabolism rockets along and always has. I can eat 2000 kcal per day no problem and I am a 47 year old woman! I have always been this way. If VLC or LC was going to slow down my metabolism or depress my thyroid (which isn't hyper either - I've had it checked twice in the last 10 years) I think it would have done so by now. Just as I can't extrapolate from my rather unusual physiology, to everybody else, neither is it possible to make blanket statements like long term VLC'ers must have slowed metabolisms. I wish!!!!
You can't say "it's simply not so" based on your rather unusual physiology. I'm only saying I would be willing to bet that on average it would be so based on the whole of animal studies, how VLC mimicks the metabolism of starvation, etc.
I will experiment with increasing metabolic flexibility more in a future after the menopausal change eventually would take place. My migraines are definitely hormone-fluctuation dependent.
After experimenting with reintroducing more carbs, I noticed the consumption of it caused less problems now than before, but I am sure I would never be like my teenager-son , or even like my husband.
Evelin,you are still eating sort-of LC,but also keeping your eyes on calories, right? Did you change something recently? I hope you will not find my question to be invasive.It just so many talks on the web about food reword and eating potatoes...
I've not changed much in the past year. I had already added in starches more regularly, mostly "safe", some not meeting PHD standards but not SAD crap. Weight has taken a back burner to other more pressing things in my life so I'm content to tread water.
I'm just making my best educated guess that VLC probably tamps down metabolic rate over time. Seems it doesn't help especially us women of a certain age in that department anyway.
You are right ... the selection bias for such a study would be hard to get around. You would have to do a randomized lengthy trial with some means of verifying compliance to a VLC diet vs. something else for several years ... I don't see that being practical.
http://www.ncbi.nlm.nih.gov/pubmed/15235325
Exercise would provide the recovery from 'metabolic derangement' that is insulin resistance. I couldn't find anything in pubmed abstracts about 'metabolic derangement' per se. I did find derangement of the metabolism of x, or the derangement of signaling pathways of y, etc. 'Derangement' just seems to mean 'impairment' or 'dysfunction.' There's no time interval attached - could be temporary, is often temporary.
I didn't mean a long term study comparing low carbers to high. What I meant was that since this experiment used 50% carb diets, the presumably healthy people should use more glucose. But, if the study used a diet of 10% carb, it's possible that now the healthy people would use more fat, and the presumably unhealthy people would be "stuck" with the same RQ [as on 50%]. This then would imply "metabolic flexibility." I'm just speculating though, and even I'm correct, I don't know which diet would keep them metabolically flexible for longer.
I didn't mean to prey, just thought you may change something in the food reword direction. I think changes should happen when the person is ready and it is obviously not the right moment for you. Probably, turning food to be more bland could require more adjustment than minimizing carbs.
One plus of being past middle-aged (for me anyways) is that motivations for losing weight related to societal pressure ease ... I am definitely hitting that old lady wearing purple stage ;).
I'm not quite sure where you're going with the FR Galina. I will say that there's lots of merit to the concept. Where I differ mostly is how that ties to setpoint, because at least on the up/gain side, such a point seems way too easy to override. I might try a low FR diet someday, but I'm of the Yoni Freedhoff school of balancing what might be optimum with what is not only livable but enjoyable. I have no desire to live a long and unsatisfying life. In that regard, most members of the calorie restriction society seem rather unhappy folk to me. No thanks!
Post a Comment
Comment Moderation is ON ... I will NOT be routinely reviewing or publishing comments at this time..