It’s high time we start treating actual DISEASE rather than risk factors anyway.
I’m currently on a personal quest to find the answers to these questions [why his lipid profile has gone from almost normal to nightmare territory after 7 years of LLVLC] and more by speaking directly with as many of my expert friends in the medical, nutrition and research fields over the next six months researching and writing my book all about this topic tentatively titled A Patient’s Guide to Understanding Your Cholesterol Test Results (releasing Fall 2013). People are so confused about what to believe about their cholesterol test results that this book is way overdue. Arming people with solid information will help them make a more informed decision about what to do about the current state of their health rather than blindly following some dubious drug therapy promoted by their doctor to treat risk factor numbers. It’s high time we start treating actual DISEASE rather than risk factors anyway.
~ Jimmy Moore
That last line really stood out to me. Mr. Moore, this whole lipid testing business grew out of the fact that for too many people, there was no treating the disease. The first indication of disease just so happened to correspond with the sort of "hard outcome" all of this is trying to avoid (or at least forestall) -- death. One thing we know for sure, autopsy findings are never helpful to the subject to improve the quality and/or length of their life. I think it's also fair to say that the shift from treating disease to prevention began with those who did manage to survive that first "event". The scientific and medical communities (including the much maligned pharmaceutical companies) have worked tirelessly to help these folks avoid a repeat. As this evolved, more and more focus was put towards identifying factors that might predispose people to develop cardiovascular disease in the first place, ways to predict early indicators of CVD progression, etc., in hopes of avoiding "the big one" entirely. In this regard, the ONLY thing we have to go on in most cases would be biomarkers, because measurable physical manifestations are usually indetectable. I know Jimmy is so very proud of his heart scan score of zero -- taken when he was like 35 years old -- but the truth of the matter is that at that age, such a score is likely meaningless, and he probably would have gotten the same score at 410 lbs a few years prior. {I realized I have used biomarkers and risk factors interchangeably, I'm not going to change that as that is generally what Jimmy is talking about anyway.}
Folks around my age and older will have meaningful first-hand memories of the saga of Jim Fixx. He's a common scapegoat for those who say you can't out-exercise a bad diet, and to large extent (but not entirely) I am in agreement. He's also a common example of a "failed ELMMer". As the Wikipedia page tells it:
James Fuller Fixx (April 23, 1932 – July 20, 1984) was the author of the 1977 best-selling book, The Complete Book of Running. Best known asJim Fixx, he is credited with helping start America's fitness revolution, popularizing the sport of running and demonstrating the health benefits of regular jogging.
On July 20, 1984, Fixx died at age 52 of a fulminant heart attack, after his daily run on Vermont Route 15 in Hardwick. The autopsy revealed that atherosclerosis had blocked one coronary artery 95%, a second 85%, and a third 70%. Although comedians remarked on the irony of dying while exercising, and there were opponents of Fixx's beliefs who said this was evidence that running was harmful, medical opinion continued to uphold the link between exercise and longevity. In 1986 exercise physiologist Kenneth Cooper published an inventory of the risk factors that might have contributed to Fixx's death. Granted access to his medical records and autopsy, and after interviewing his friends and family, Cooper concluded that Fixx was genetically predisposed (his father died of a heart attack at age 43 and Fixx himself had a congenitally enlarged heart), and had several lifestyle issues. Fixx was a heavy smoker prior to beginning running at age 36, he had a stressful occupation, he had undergone a second divorce, and his weight before he took up running had ballooned to 220 pounds (100 kg).
Vegetarians and others focused on Fixx's consumption of steaks and such, and he was probably the quintessential example upholding the lipid hypothesis. Although he had a congenital heart issue, his blockages were what "caused" his death, thus the blame traces back to what caused the blockages. IMO, far too much has always been made over the circumstances of one man's health/death. It's not unlike that of Dr. Atkins. However what is good for the goose is good for the gander, and personally I find the mystery over Atkins autopsy troubling because of this. We should all resist the temptation to draw conclusions over a single individual's experience, but this is why scientific studies are done ... and where there are no studies? ... we look to epidemiological population studies (by that I mean populations on the whole more than at dietary intakes within populations such as meat eaters vs. vegetarians ).
In any case, I'm also old enough to have grown up through this evolution in healthcare from treating disease once it has manifested to "treating risk factors". This approach is more accurately described as an effort to identify a pathological progression in the early stages, long before disease technically presents. Preventative vs. symptomatic intervention vs. palliative medicine. It is fair to say that such changes have brought about improved outcomes for health/disease in some areas more than others. I do not intend to, nor could I even if I were so inclined, discuss some comprehensive accounting of this. As a young adult, blood pressure screening was NOT a matter of routine. Sure, if I went for an annual physical or somesuch, yes, but if I went for a scratchy throat or sprained ankle? Nope. Now you can't even go to a walk-in for a physical injury (such as slicing off a small sliver of a fingertip with a mandolin) without weighing in and getting your BP checked. Why? Because elevated blood pressure was identified as a risk factor for CVD, and somewhere along the line it was decided that measuring this seemingly randomly might be a good idea to catch the early warning. After all, almost nobody feels modestly elevated BP, and yet if one has chronically elevated BP there's pretty much the closest thing to a unanimous concensus as there can be that something negative is causing this.
Isn't this what the whole obsession in the low carb community with blood glucose levels amounts to? So people don't get diagnosed with diabetes years, sometimes decades, after the etiological precursors have already wrought unquantifiable damage? This folks is the problem with the advocates of low carb. They fixate on glucose levels to the utter ignorance of most lipids and virtually everything else. Not to mention that when it comes to biomarkers, the cherry picking season lasts year round in LLVLC-land. One cannot say one parameter is meaningless and another is all that matters based on personal preference. Biomarkers can't only matter when they are in favor of a lifestyle you advocate, but become meaningless when they run counter to it.
So now I'm going to do something I don't often do ... cut Jimmy a little slack. Because what I think he meant to say was that it's time we treated disease instead of symptoms -- more specifically identify what's causing the problem and work on correcting that rather than just putting bandaids on the problems. Ironically, however, this is one of the very issues I have with how LC Dogma addresses hyperglycemia, because hyperglycemia is not the cause of diabetes, it is a symptom. But there is an analogy to lipids in the glycemia picture as well. Glucose metabolism doesn't need to go totally haywire to hint at underlying problems in the making. Jimmy are you paying attention? Rising fasting glucose levels or lingering elevated postprandial levels are BIOMARKERS. There is little evidence that such glucose levels in and of themselves are "disease" ... there's pretty much a predominance of evidence that these glucose levels are symptoms of underlying issues.
So too, are lipoprotein levels. We can argue about which ones are more important, good, bad, indifferent. We can argue which measurement is the better biomarker. But lipoprotein levels are CLEARLY significant players in this realm. If one accepts that eating X diet lowers glucose and insulin levels and all the implications thereof, one must also accept that if X raises LDL, this cannot be ignored. This is not to mention how the LC community all but ignores free fatty acids ... it's the forgotten lipid!
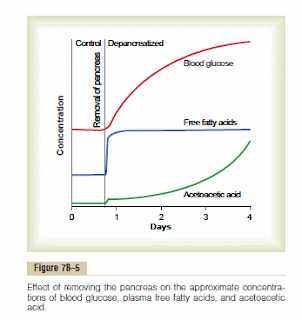 The scientific literature is pretty clear and consistent in indicating that the fatty acid metabolism goes wonky (how's that for sciencey talk) first. The figure at right is from Guyton & Hall Textbook of Medical Physiology and shows starkly just how fast this happens when you remove an animal's pancreas. The free fatty acids jump right up almost instantly, and the concentration levels off. It takes a few days for the blood glucose (presumably these are average levels) to climb and it appears to level off, presumably at the limits of gluconeogenesis. The acetoacetic acid -- ketones -- are on the rise and continue to climb following an accelerating trajectory. This is what ultimately kills these animals, not hyperglycemia, or, to be fair, the fatty acids per se, but the ketones come from the excessive fattty acids.
The scientific literature is pretty clear and consistent in indicating that the fatty acid metabolism goes wonky (how's that for sciencey talk) first. The figure at right is from Guyton & Hall Textbook of Medical Physiology and shows starkly just how fast this happens when you remove an animal's pancreas. The free fatty acids jump right up almost instantly, and the concentration levels off. It takes a few days for the blood glucose (presumably these are average levels) to climb and it appears to level off, presumably at the limits of gluconeogenesis. The acetoacetic acid -- ketones -- are on the rise and continue to climb following an accelerating trajectory. This is what ultimately kills these animals, not hyperglycemia, or, to be fair, the fatty acids per se, but the ketones come from the excessive fattty acids.
In terms of diabetes, what the advocates of low carb diets for managing hyperglycemia are ultimately doing is treating the symptom and not the disease. In the case of your classic obese insulin resistant person, FBG and 2hr OGTT glucose levels are no more or less biomarkers than fasting lipids. If Jimmy's point is that the first line of defense should be nutritional, and not pharmaceutical, I agree ... and you know what? It is reckless hyperbole to insinuate that the vast majority of doctors don't also agree. But when lifestyle intervention does not produce results, they are NOT "treating biomarkers", they are at least attempting to treat the underlying disease so that it doesn't progress.
Truly effective therapies correct what is actually causing the problem. There is legitimate argument as to whether statins, oral hypoglycemics, etc. actually do that, but this is the goal of pharmaceutical intervention ... or it should be.
As Jimmy Moore continues his quest to solve his medical mysteries, he is making a mockery of low carb, therapeutic ketogenic diets and, it seems, Paleo seems determined to go along for the ride. There is no way to interpret his latest lipids other than that they are an utter disaster. In the comments on his post he was asked why he changed what was working for him in 2005, and he stays firm that it stopped working for him. Not so, according to his 2007 resolutions. His October 2005 lipids were long enough post his 2004 weight loss that they are "real" maintenance levels. He's now back to hanging his hat on Mary Vernon's assurances that weight loss throws lipids all outta whack and are not to be trusted. I will agree to some extent, but it is rare to see such a dramatic worsening in the face of weight loss. No ... in 2006, and continuing on through 2007 and beyond, what Jimmy did in 2004-5 that was working, didn't stop working. HE STOPPED WORKING IT. Looking to his example and you have a classic case of how exercise really does factor into all of this after all. In 2005 he engaged in good-old-fashioned cardio -- 45 min-1 hour nearly daily. In 2006 he admitted to slacking off and there were weight gains involved. Not huge ones, but his worsening lipids no doubt coincided with his reduced activity and who knows what other dietary changes were involved. This man is so coy and prone to exaggeration or minimization (whichever suits his purpose) it is hard to tell, but I'll bet he was eating quite rather differently than 2004-5. But I didn't really mean to go off on a tangent here ...
I go back and forth about various biomarkers. For starters, there is just so much confusion as to what counts and why -- as the awesome conversations we've been having in the comments here clearly demonstrate. Here is my bottom line, however. If MY biomarkers improve, then I'm doing something right. If MY biomarkers deteriorate, then I'm doing something wrong. I am sure Jimmy Moore feels great right now. How much of that is secondary to the support and adulation he's receiving for losing weight again? It surely is preventing him from taking a long hard look at those numbers on the paper, and what Dr. Dayspring is saying about them. It's not just Dayspring. This LDL-P stuff is pretty well accepted by the scientific community even if they don't all agree on what causes it and/or what to do about it. Still, there's no one single lipid profile, and if Jimmy and most LC'ers tell us anything, the fasting triglycerides may well only be of importance in the context of a mixed diet.
Bottom line:
Jimmy Moore ignoring horrendous LDL-P and Apo-B levels -- that worsened with weight loss on his (absurd) diet -- is no better than would be a Harley Johnstone (aka Durian Rider) ignoring fasting blood glucose on the rise through the years. Period. He seems bound and determined to convince himself that his lipid profile -- worse now than at 410 lbs!!! -- is some how irrelevant in the context of a ketogenic diet. I.T. I.S. N.O.T. Does he seriously think this will improve if/when he stabilizes out and maintains his weight loss? Perhaps if he loses considerably more weight.
Speaking of Durian Rider, he posted his own 2 year lipid results on YouTube, though not nearly as detailed as Jimmy.
In closing ... Biomarkers/Risk Factors ARE attempting to unveil underlying disease before it has progressed irreversibly or manifested itself in truly deleterious fashion or death. It is imperfect. I don't think we all need to obsess over it all the time either. Risk is just that ... risk. We all know someone who smoked like a chimney and lived to a ripe old age when they died of natural causes, and we know of those who lived a healthy life that died young. This is the whole "X number of folks who have heart attacks had low/normal LDL" thing continues to be all about. Based on that, Dana Reeve's death from lung cancer refutes the "tobacco hypothesis" that smoking increases lung cancer risk. No. And I think this is ultimately Dayspring's point in Jimmy's comment section. His LDL-C is so high, there is no question in anyone's mind that the LDL-P and Apo-B would be high ... and they are. Jimmy needs only to be honest with himself, return to his 2005 lifestyle, and I have no doubt he would return to more normal lipids that could be justified. What he's trying to rationalize now is, indeed, insanity.
So now I'm going to do something I don't often do ... cut Jimmy a little slack. Because what I think he meant to say was that it's time we treated disease instead of symptoms -- more specifically identify what's causing the problem and work on correcting that rather than just putting bandaids on the problems. Ironically, however, this is one of the very issues I have with how LC Dogma addresses hyperglycemia, because hyperglycemia is not the cause of diabetes, it is a symptom. But there is an analogy to lipids in the glycemia picture as well. Glucose metabolism doesn't need to go totally haywire to hint at underlying problems in the making. Jimmy are you paying attention? Rising fasting glucose levels or lingering elevated postprandial levels are BIOMARKERS. There is little evidence that such glucose levels in and of themselves are "disease" ... there's pretty much a predominance of evidence that these glucose levels are symptoms of underlying issues.
So too, are lipoprotein levels. We can argue about which ones are more important, good, bad, indifferent. We can argue which measurement is the better biomarker. But lipoprotein levels are CLEARLY significant players in this realm. If one accepts that eating X diet lowers glucose and insulin levels and all the implications thereof, one must also accept that if X raises LDL, this cannot be ignored. This is not to mention how the LC community all but ignores free fatty acids ... it's the forgotten lipid!
 The scientific literature is pretty clear and consistent in indicating that the fatty acid metabolism goes wonky (how's that for sciencey talk) first. The figure at right is from Guyton & Hall Textbook of Medical Physiology and shows starkly just how fast this happens when you remove an animal's pancreas. The free fatty acids jump right up almost instantly, and the concentration levels off. It takes a few days for the blood glucose (presumably these are average levels) to climb and it appears to level off, presumably at the limits of gluconeogenesis. The acetoacetic acid -- ketones -- are on the rise and continue to climb following an accelerating trajectory. This is what ultimately kills these animals, not hyperglycemia, or, to be fair, the fatty acids per se, but the ketones come from the excessive fattty acids.
The scientific literature is pretty clear and consistent in indicating that the fatty acid metabolism goes wonky (how's that for sciencey talk) first. The figure at right is from Guyton & Hall Textbook of Medical Physiology and shows starkly just how fast this happens when you remove an animal's pancreas. The free fatty acids jump right up almost instantly, and the concentration levels off. It takes a few days for the blood glucose (presumably these are average levels) to climb and it appears to level off, presumably at the limits of gluconeogenesis. The acetoacetic acid -- ketones -- are on the rise and continue to climb following an accelerating trajectory. This is what ultimately kills these animals, not hyperglycemia, or, to be fair, the fatty acids per se, but the ketones come from the excessive fattty acids.In terms of diabetes, what the advocates of low carb diets for managing hyperglycemia are ultimately doing is treating the symptom and not the disease. In the case of your classic obese insulin resistant person, FBG and 2hr OGTT glucose levels are no more or less biomarkers than fasting lipids. If Jimmy's point is that the first line of defense should be nutritional, and not pharmaceutical, I agree ... and you know what? It is reckless hyperbole to insinuate that the vast majority of doctors don't also agree. But when lifestyle intervention does not produce results, they are NOT "treating biomarkers", they are at least attempting to treat the underlying disease so that it doesn't progress.
Truly effective therapies correct what is actually causing the problem. There is legitimate argument as to whether statins, oral hypoglycemics, etc. actually do that, but this is the goal of pharmaceutical intervention ... or it should be.
As Jimmy Moore continues his quest to solve his medical mysteries, he is making a mockery of low carb, therapeutic ketogenic diets and, it seems, Paleo seems determined to go along for the ride. There is no way to interpret his latest lipids other than that they are an utter disaster. In the comments on his post he was asked why he changed what was working for him in 2005, and he stays firm that it stopped working for him. Not so, according to his 2007 resolutions. His October 2005 lipids were long enough post his 2004 weight loss that they are "real" maintenance levels. He's now back to hanging his hat on Mary Vernon's assurances that weight loss throws lipids all outta whack and are not to be trusted. I will agree to some extent, but it is rare to see such a dramatic worsening in the face of weight loss. No ... in 2006, and continuing on through 2007 and beyond, what Jimmy did in 2004-5 that was working, didn't stop working. HE STOPPED WORKING IT. Looking to his example and you have a classic case of how exercise really does factor into all of this after all. In 2005 he engaged in good-old-fashioned cardio -- 45 min-1 hour nearly daily. In 2006 he admitted to slacking off and there were weight gains involved. Not huge ones, but his worsening lipids no doubt coincided with his reduced activity and who knows what other dietary changes were involved. This man is so coy and prone to exaggeration or minimization (whichever suits his purpose) it is hard to tell, but I'll bet he was eating quite rather differently than 2004-5. But I didn't really mean to go off on a tangent here ...
I go back and forth about various biomarkers. For starters, there is just so much confusion as to what counts and why -- as the awesome conversations we've been having in the comments here clearly demonstrate. Here is my bottom line, however. If MY biomarkers improve, then I'm doing something right. If MY biomarkers deteriorate, then I'm doing something wrong. I am sure Jimmy Moore feels great right now. How much of that is secondary to the support and adulation he's receiving for losing weight again? It surely is preventing him from taking a long hard look at those numbers on the paper, and what Dr. Dayspring is saying about them. It's not just Dayspring. This LDL-P stuff is pretty well accepted by the scientific community even if they don't all agree on what causes it and/or what to do about it. Still, there's no one single lipid profile, and if Jimmy and most LC'ers tell us anything, the fasting triglycerides may well only be of importance in the context of a mixed diet.
Bottom line:
Jimmy Moore ignoring horrendous LDL-P and Apo-B levels -- that worsened with weight loss on his (absurd) diet -- is no better than would be a Harley Johnstone (aka Durian Rider) ignoring fasting blood glucose on the rise through the years. Period. He seems bound and determined to convince himself that his lipid profile -- worse now than at 410 lbs!!! -- is some how irrelevant in the context of a ketogenic diet. I.T. I.S. N.O.T. Does he seriously think this will improve if/when he stabilizes out and maintains his weight loss? Perhaps if he loses considerably more weight.
Speaking of Durian Rider, he posted his own 2 year lipid results on YouTube, though not nearly as detailed as Jimmy.
5/4/09 Blood workTriglycerides = 0.6 mmol/l = 53 mg/dlTC = 3.5 mmol/l = 135 mg/dlHDL = 1.3 mmol/l = 50 mg/dlLDL (Calculated) = 1.9 mmol/l = 73 mg/dl
5/17/2011 Blood workTriglycerides = 0.7 mmol/l = 62 mg/dlTC = 4.8 mmol/l = 186 mg/dlHDL = 1.5 mmol/l = 58 mg/dlLDL (Calculated) = 3 mmol/l = 116 mg/dlSeems Harley's lipids have ticked up slightly, and woopsey, whassup widdat LDL there? But according to Dayspring, he's quite close to that 1:1 Trig:HDL ratio. Absent an abominable LDL level, it looks like there's not much cause for concern (I'd be concerned for myself if a repeat test showed progression, that's almost a 60% increase in two years, not inconsequential!!). But that's the same Trig:HDL ratio Jimmy hangs his hat on.
In closing ... Biomarkers/Risk Factors ARE attempting to unveil underlying disease before it has progressed irreversibly or manifested itself in truly deleterious fashion or death. It is imperfect. I don't think we all need to obsess over it all the time either. Risk is just that ... risk. We all know someone who smoked like a chimney and lived to a ripe old age when they died of natural causes, and we know of those who lived a healthy life that died young. This is the whole "X number of folks who have heart attacks had low/normal LDL" thing continues to be all about. Based on that, Dana Reeve's death from lung cancer refutes the "tobacco hypothesis" that smoking increases lung cancer risk. No. And I think this is ultimately Dayspring's point in Jimmy's comment section. His LDL-C is so high, there is no question in anyone's mind that the LDL-P and Apo-B would be high ... and they are. Jimmy needs only to be honest with himself, return to his 2005 lifestyle, and I have no doubt he would return to more normal lipids that could be justified. What he's trying to rationalize now is, indeed, insanity.
Comments
From where I stand, Durain looks like his lipids are improving. If they hold near where they are now, he has reduced his risk of cancer, sepsis, or even, amazingly, mental illness.
CVD is not the only death in town and low lipids can point to other risks. Weakly, as always - a high or low lipid count (extreme extremes aside) is not as alarming as a positive biopsy, or even an abnormal blood pressure check. But you are right that trends over time mean something.
A 'reverse epidemiology' of cardiovascular risk is observed in chronic kidney disease, chronic heart failure, chronic obstructive lung disease, cancer, AIDS and rheumatoid arthritis, and in the elderly. These populations apparently have slowly progressive to full-blown wasting and significantly greater short-term mortality than the general population. The survival paradoxes may result from the time differential between the two competing risk factors [i.e. over-nutrition (long-term killer but short-term protective) versus undernutrition (short-term killer)]. Hemodynamic stability of obesity, protective adipokine profile, endotoxin-lipoprotein interaction, toxin sequestration of fat, antioxidation of muscle, reverse causation, and survival selection may also contribute.
Also, what of oxLDL?
http://diabetes.diabetesjournals.org/content/54/5/1506.full
Linoleic Acid Increases Lectin-Like Oxidized LDL Receptor-1 (LOX-1) Expression in Human Aortic Endothelial Cells
If you lower LDL by a method that increases oxLDL, have you gained?
Not if this is the result:
http://www.ncbi.nlm.nih.gov/pubmed/8960090
Israel has one of the highest dietary polyunsaturated/saturated fat ratios in the world; the consumption of omega-6 polyunsaturated fatty acids (PUFA) is about 8% higher than in the USA, and 10-12% higher than in most European countries. In fact, Israeli Jews may be regarded as a population-based dietary experiment of the effect of a high omega-6 PUFA diet, a diet that until recently was widely recommended. Despite such national habits, there is paradoxically a high prevalence of cardiovascular diseases, hypertension, non-insulin-dependent diabetes mellitus and obesity-all diseases that are associated with hyperinsulinemia (HI) and insulin resistance (IR), and grouped together as the insulin resistance syndrome or syndrome X. There is also an increased cancer incidence and mortality rate, especially in women, compared with western countries. Studies suggest that high omega-6 linoleic acid consumption might aggravate HI and IR, in addition to being a substrate for lipid peroxidation and free radical formation. Thus, rather than being beneficial, high omega-6 PUFA diets may have some long-term side effects, within the cluster of hyperinsulinemia, atherosclerosis and tumorigenesis.
Statins are thought to be LOX-1 inhibitors,
but then so are some herbals and foods.
'Cancer death rates for Israeli Arabs, who consumed a more traditional Mediterranean diet - more monounsaturated fatty acids, mostly olive oil, and less n-6 polyunsaturated fatty acids - are still 1.1-1.7 times (men-women) lower than in Israeli Jews, but are increasing faster (23.6 and 5.1% vs. 5.3 and -3.3%, 1980-2000), concurrently with dietary 'Israelization' - specifically, increased intake of n-6 polyunsaturated fatty acids. Israeli-Jewish women attained an earlier, much larger (29 vs. 7%, 1999) 'cancer : heart disease mortality shift' (ratio >1.0), ranked much worse for cancer (15th/44 European countries) than men (37th) and heart disease (38th and 34th, respectively), and had much higher cancer prevalence (1 : 3) than Israeli-Arab women (1 : 6), though dietary compositions were similar, save for higher n-6 polyunsaturated fatty acid and polyunsaturated fatty acid : monounsaturated fatty acid ratio. '
Each of the sides cites studies and anecdotal reports to support what they are selling, it's not too surprising that a person who is actively trying to improve his/her health/appearance/quality of life will see some benefit regardless of the method.
If I told you that you had to eat only beans on toast while riding a unicycle and a total of 100 people "bought into" the beans/toast/unicycle method a few of them would enjoy tremendous results, on account of they are eating beans on toast while riding a unicycle.
It's really not all that different being a television psychic who engages in "cold reading," out of 20 readings you are going to have say 3 where you happen to get some hits.
Get 20 people to sit on a block of ice for 15 minutes a day, after two months 3 of the 20 have improved lipids or have lost a few pounds which is entirely coincidental and you can proclaim "This is why the medical establishment fears me!"
Is there any diagnostic we can all agree on?
How long someone can hold their breath for?
If it gets longer, they're getting healthier, if shorter, they're getting worse...
Atkins? I believe he was the doctor, not the patient. Nor do I remember him posting much in the way of personal health statistics in his books.
He may have struggled to follow his own best advice, like most of us.
His diet followed "dietary guidelines" when it came to PUFA/SFA, and his supplement protocols seem dated and heavy-handed today, but were typical of his time.
After a 12-h fast, 10 healthy young men ingested mixed meals containing 0 g (control) or 40 g fat, provided as butter, olive oil or sunflower oil in a random order. Fasting and postmeal blood samples were collected for 7 h. The no-fat test meal did not elicit any change over baseline except for plasma phospholipids, insulin and nonesterified fatty acids. Conversely, the three fat-containing meals elicited bell-shaped postprandial changes (P < 0.05) in serum triacylglycerols, free and esterified cholesterol, and nonesterified fatty acids. The butter meal induced a lower postprandial rise of triacylglycerols in serum and chylomicrons (incremental AUC, mmol.h/L: 0.72) than the two unsaturated oils (olive oil: 1.6, sunflower oil: 1.8), which did not differ. Circulating chylomicrons were smaller after the butter meal than after the two vegetable oil meals. The in vitro susceptibility of circulating chylomicrons to hydrolysis by postheparin plasma was higher after sunflower oil than after butter or olive oil. We conclude that butter results in lower postprandial lipemia and chylomicron accumulation in the circulation of young men than olive or sunflower oils after consumption of a single mixed meal.
Are smaller chylomicrons a good thing? What's this about then?
By multivariate analysis, HCV infection was independently associated with diabetes only in subjects without hyperlipidemia (defined as triglycerides above 150 mg/dL and/or total cholesterol above 200 mg/dL; adjusted odds ratio 1.35, 95% CI 1.17–1.55) but not in those with hyperlipidemia. Among patients with diabetes, anti-HCV was positive in 7.3% of those with hyperlipidemia and 22.4% of those without (P < 0.001). Hypertriglyceridemia occurred in 31.4% of HCV-infected patients and 53.8% of non-infected patients (P < 0.001), and hypercholesterolemia occurred in 34.7% and 60.1%, respectively (P < 0.001).
The lack of association between HCV infection and diabetes in subjects with hyperlipidemia in Liu’s study may partly be explained by a difference in viral activity. Hyperlipidemia may be a surrogate marker of low HCV RNA. These patients are less likely to have HCV-associated diabetes.
Diabetes is associated with cirrhosis and hepatocellular carcinoma (HCC) in patients with chronic hepatitis C. In a community study of 23 820 Taiwan residents, the relative risk of HCC in non-diabetic chronic hepatitis C patients was 15.0 (95% CI 10.0–22.5) compared to subjects without HCV infection, and the relative risk in diabetic patients with chronic hepatitis C further increased to 60.3 (95% CI 23.6–153.6).[7] Similarly, chronic hepatitis C patients with body mass index ≥ 30 kg/m2 were more likely to develop HCC than non-obese subjects without HCV infection (relative risk 34.5; 95% CI 13.5–87.6). In another study of 248 patients with compensated HCV cirrhosis, insulin resistance was independently associated with HCC development.[8] Insulin resistance also increased the risk of liver-related death and the need for liver transplantation.
On the other hand, despite the positive correlation with diabetes, HCV infection does not appear to increase the risk of cardiovascular morbidity and mortality.[9] Similarly, carotid intima-media thickness is not increased in patients with chronic hepatitis C.[10] Atherosclerosis is associated with metabolic risk factors instead of HCV infection. One possible explanation is that the harmful effect of diabetes is partially offset by the more favorable lipid profile in chronic hepatitis C patients.
http://beforeitsnews.com/healthcare/2012/11/hepatitis-c-virus-infection-and-diabetes-not-a-straightforward-relationship-2443048.html
(however, I've seen another paper recently that does correlate HCV with death from circulatory causes - AHR 1.50 - but some of this small effect may be due to a) circulating immune complexes damaging circulation in patients with cryoglobulinaemia b) poor blood clotting due to cirrhosis, rather than lipids. http://www.hcvsociety.org/forum/viewtopic.php?f=31&t=529 )
One unintended consequence of LookAHEAD is that it shows treating risks is working! The "hard outcome" rates were so much lower than expected to begin with.
As to Atkins, he mentioned his own weight loss and glorified many successes in his books. My copy of the original has temporarily gone missing, but there is the story of that workplace intervention where all but one of the subjects lost all of their excess weight, that one still losing a lot of weight, and keeping it off. Dr. Eades is another who mentions his own weight loss and has profited from pie-in-the-sky rhetoric in his books on effortless weight loss and the glories of LC. Yet he needs to wear girdles and hide behind a bench while hawking his sous vide.
I think when you are the doctor who has been your own patient, you are every bit as accountable as any run of the mill weight loss success story, etc. Atkins was rather sanctimonious in his bucking against the establishment, so if his is the better way, show me the money, right?
My current belief is that LC is an excellent option for weight loss, but not an appropriate diet in maintenance for a number of reasons. Ketogenic diets have legitimate therapeutic applications, but there are trade-offs, and there is just scarce little information out there on the long-term effects of such diets. I would also note that most keto diets are also calorie restricted.
We also don't know if James Fuller Fixx had died even earlier had he not done any exercise.
I've also never seen an experiment where a group of patients who were so sick that they did not like any exercise were forced to do so any how and, low and behold, lived longer.
PLoS One. 2012;7(5):e37887. doi: 10.1371/journal.pone.0037887.
Adverse metabolic response to regular exercise: is it a rare or common occurrence?
Individuals differ in the response to regular exercise. Whether there are people who experience adverse changes in cardiovascular and diabetes risk factors has never been addressed.
Numbers of adverse responders reached 12.2% for SBP, 10.4% for TG, and 13.3% for HDL-C. About 7% of participants experienced adverse responses in two or more risk factors.
Adverse responses to regular exercise in cardiovascular and diabetes risk factors occur.
PMID: 22666405
' The prevalence of ARs appears to be similar at low and high doses of exercise. However, we do not know whether some adverse responders would revert to a more positive response pattern if exposed to different exercise doses or exercise modalities.'
Yep.
Having said all that, I think it's very likely that Moore's thyroid has been driven into the dirt by his yo-yo dieting, thus leading or contributing to his high cholesterol. I was a slim, active, 26-year-old woman with high cholesterol because of hypothyroidism-- it dropped 80 pts when I upped my synthroid. Granted, I would be shocked that his doctors have not investigated this. Still there's the controversial Type 2 Hypothyroidism which Dr. Atkins, himself, believes is a possible consequence of LC'ing or any long term dieting.
Post a Comment
Comment Moderation is ON ... I will NOT be routinely reviewing or publishing comments at this time..