Jimmy Moore's Cholesterol Clarity ~ Ongoing Review and Information ~ Most Recent Update 9/19/13
The original opening to this post can be read by scrolling to the end or using your browser search function to find ##### .
The intent of a single post is that for as long as this content is relevant, I will add new information to this post and "bump" it to the top of the feed. If it grows to be unmanageable, I'll have sections with search strings for easy navigation. For now, each update will get popped to the top of the feed reader. New "entries" will be at the top, and will be separated from prior content with "▼▼ Content added XX/XX/XX ▼▼". Different topics within each update will be separated by ***** and a horizontal line ... like this:
***** ▼▼ Content added 9/19/13 ▼▼
Interpreting Cholesterol Panels?
The final chapter of this book contains a series of 30 lipid and other marker profiles. They are mixed up and this is presented as a means of doing some practical application of the information in the book.
Your mission (if you choose to accept it) is to interpret them based on everything you’ve learned. See if you can identify those with healthy results, those who could stand to improve their numbers, and those who have poor health risk markers.
Now, some are taking meds, there's a diabetic, some taking meds (statins or other) and a few with genetic markers, etc. so there's no way to really do any sort of fair appraisal. I skipped this entirely when I read the book, but something prompted me to give it a second look. So I took the liberty of summarizing the results for TC, LDL, HDL, trigs, and LDL-P for all but one example where LDL and TC were missing. I included the ApoB on the three where it was included but left off the rest. I wanted to summarize as much for the parameters reported for all. Also, in the book Chris Masterjohn (and others) discussed the TC/HDL ratio being important as well as non-HDL-C. The latter tracks well with ApoB. In the book Chris did not put a number on this to shoot for, but one of Jimmy's experts, Dr. Davis, puts the goal at under 130 (hat tip Charles Grashow). As for the TC/HDL, a cut-off of 3 is generally thrown around, keeping in mind that a "high end normal" TC and usual HDL would give a ratio of 4.
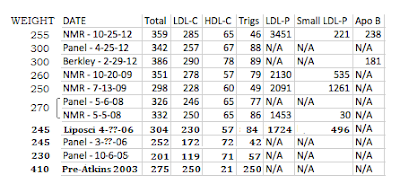
So, here are the profiles.
The top row is "healthy markers". I kid you not. You have five profiles there with TC around or above 300 and one exceeding 400 (which Jimmy Moore's has more recently as well). You have one LDL exceeding 300 and one pretty close, and five that are near or over 200. While the HDL's are high in some, most are pretty "normal" so they aren't pulling most of these folks out of the risk-fire. Considering that one of the experts you "learn from" in the book is Dr. Dayspring, I think his guidelines (in addition to Davis') are interesting to note here. For all the grumblings over triglycerides, Dayspring's #1 addresses them first if over 500. The 400-500 threshold is pretty common and, while it may need to be addressed in light of LDL-P, look at the segment in the middle row-left. Those 8 profiles are deemed "some work needed", as opposed to those above them and it is clear that Jimmy determines this with the arbitrary benchmark of triglycerides over 100. Keep in mind that 150 is the high end of normal that is generally accepted and only one of the six skirts close to that. If Jimmy wants to say that LDL-P matters, then he's got a tough time of it justifying himself as "healthy" - small LDL-P not being recognized as a reliable marker the context of his astronomical LDL-P.
Now it is of interest here that you have high LDL-P in this group with normal trigs, but most have elevated LDL and TC. I have no quarrel with the "poor" designees (middle right block) except it is interesting to note that their trigs are higher without much more elevated LDL-P compared to the middle group. Indeed looking at all of these -- including that outlier there in the upper right, which would be Jimmy -- LDL-P and triglycerides don't seem to track with one another. Jimmy Moore and a few doctors have arbitrarily chosen triglycerides as the marker "that matters", but as I intend to show in an upcoming post, they are probably picking the long odds marker here.
In any case, none of these have "immediate attention required" trigs per Dayspring so we proceed to #2 on his list:
2) Look at the LDL-C, because if it is above 190 mg/dL, drug therapy is indicated no matter what else you find. At lesser levels it depends on the risk of the patient whether drug treatment is indicated.Five of fourteen "healthy" folks meet this criterion, and a sixth comes within a couple of points. By contrast, nobody in the "some work needed" or "poor" categories meet this. I should have included gender, but all but one of the "poor" meet this criterion. And then there's the TC/HDL ratio under 4. You have two healthy and four middle group that exceed this. Dayspring also puts non-HDL-C at 130 and ten of the healthy people fail here! Many by quite a lot, not just a little bit. The healthy are certainly less so compared to those that need work again by this parameter.
Did Westman read this section? Did he offer up any Doctor's Notes? The answer to the second question is NO. I ask why not?
Jimmy definitively quizzes readers and concludes he is healthy because of "markers that matter" -- to him. Nevermind ALL OF THE SCIENTIFIC RESEARCH that counters his conclusions. This is why this book is downright dangerous if you ask me.
Here's a simple question to ask any of these LC docs and let's see if they'll answer it: Would a ketogenic diet protect a person who is homozygous for familial hypercholesterolemia? As in would lowering triglycerides and/or raising HDL improve their outcome or negate their very-high LDL? I think we know the answer to that but I also doubt we'll hear it voiced by any of these folks.
What's that block in the lower left? Well just for reference I included the two case studies in Robb Wolf's Reno first responders study paper. On the left are the "before" profiles (Case 1 and 2), and on the right "after". It is worth noting that both cases involved statins with no mention of "titrating off" or miniscule doses, and Case 1 involved undisclosed "more pharmaceuticals". Do you notice anything? First off, Case 1 is likely not LC and yet a case could be made that he bests most of the "healthy" markers in Jimmy's book. Case 2 didn't look all that bad in the lipids department to begin with except for the HDL which came up to a respectable level -- while LDL-P went DOWN.
I suspect that this is one reason Robb Wolf ultimately either wasn't interviewed for the book or wasn't included, though I'm not sure who did the ultimate declining there. I also suspect this is but one reason why Robb hasn't joined the parade of 5 Star reviews over on Amazon.
***** ▼▼ Content added 9/8/13 ▼▼
Familial Hypercholesterolemia
Chapter 14 Nine Reasons Why Cholesterol Levels Can Go Up, Topic 4, p. 151
Jimmy writes:
I was surprised the first time FH was indicated on my cholesterol test results. So when I decided to write Cholesterol Clarity I figured I’d take the plunge and get tested for it. Was my high total cholesterol that has been in excess of 400 at times due to FH or something else? In April 2013, I paid $1,200 to Ambry Genetics (Ambrygen.com/tests/familial-hypercholesterolemia) and the results would probably surprise the cardiologist whose note is reprinted above: According to my LDLR and ApoB genes, I have a “significantly decreased likelihood” of FH.
This was a wasted $1200. As Jackie Eberstein had pointed out to him years ago, having a normal lipid panel in October 2005 pretty much took genetics out of the picture. Jimmy Moore is 41 y.o. and this sort of thing is likely not first diagnosed at his "advanced age" (for the condition). But here is a quote that I consider to be one of THE most irresponsible things I've read in this book that is chock full of irresponsibility:
Dr. Jeffry Gerber, who assisted me with getting this test run, confirmed that “the results are most favorable for you. May your LDL-P continue to rise and may you live a long and healthy life.”

Was this said in jest? Maybe?? Although I cannot see why a doctor would joke about such a thing. The graphic at right, from this analysis of Framingham study data, is pretty damning of LDL-P.
Why would anyone wish someone's LDL-P to continue to rise? Or even stay as is?
I think this also brings Westman's co-author role into question. In his podcast interview with Diane Sanfillipo Jimmy pretty much describes Westman's input as after the fact comments. Those "Doctor's Notes". None here in this chapter. Did Westman read Gerber's comments? No alarm there?
In this section Jimmy again quotes Dr. Dayspring:
“Cholesterol in the blood might correlate with heart disease in a population, but it can never be used by individual patients because of the propensity for discordance between cholesterol and atherogenic particle measurements. It takes cholesterol getting into the artery wall to kill you. And because all lipids—including cholesterol and triglycerides—are trafficked as passengers inside the lipoprotein, it’s the type, the number, the quality of the lipoproteins that determine whether the little dump truck [lipoprotein] carrying the cholesterol molecules is going to invade your artery wall or not.”
Unlike many of Jimmy's experts, Dayspring is/was familiar with Jimmy Moore's lipid profile and diet. He called it a "nightmare" and specifically suggested to him that he try reducing saturated fat in his diet, and if that failed that he should consider statins. Those aware of Dayspring's views know that the bolded part is referring to apoB "tagged" LDL particles.
*****
My Review on Amazon
I will probably be doing a separate post on the fall-out from this review. Here is the link. The comments on my review and one left by Dorothy Brewster are enlightening to say the least.
Upon seeing the cover of this book, many people may get excited ... Finally a book for us patients that can help sort out some of the issues that arise when that lipid panel comes back from the lab, complete with the scary risk notations in the margin. Such a book is sorely needed. This is not that book.
Jimmy Moore has missed a golden opportunity to truly help educate people on the controversies and the current consensus on the significance (or lack thereof) of the various biomarkers and measures for assessing cardiovascular risk. This is evident in that one of the most controversial and important topics of the day in lipidology -- LDL particle number vs. LDL particle size -- is all but avoided in the one chapter devoted to the topic. This is such a disservice to those who might recognize the names of Dr. Thomas Dayspring and Dr. Ronald Krauss and purchase this book in hopes of learning more from them. Save your money.
Instead of engaging Krauss and Dayspring (and a few other true experts interviewed for the book) in a genuine dialog, Jimmy Moore has reduced this important and complex topic to a series of sound bite-style quotations (called Moments of Clarity), cobbled together with his highly biased commentary, and finished off with often banal Doctor's Notes from co-author Dr. Eric Westman. What value there is, in some of the sound bites, is diluted with quotes from "experts" with absolutely no qualifications or knowledge to be designated as such. Most are merely known within the low carb internet community and have perhaps been a guest on one of the author's podcasts.
Let's say there is a major capital improvement initiative under consideration in your town. The stakes are high and the outcome, one way or the other, will impact you personally for decades to come. Would you want to base your decision on the 30 second commercials put forth by political interest groups? Worse yet, on only those commercials a biased media outlet chose to carry? Of course not. You would attend the town hall meeting. Jimmy Moore could have brought you this town hall meeting. Instead he is the biased media outlet bringing you sound bites.
If you have troublesome cholesterol levels and want a book to convince you there's absolutely nothing to worry about, this is the book for you. If you want unbiased information to assist you to work *with* your doctor, this is not the book for you.
You will get far more information from two interviews Krauss did with meandmydiabetes: LDL Cholesterol - Ron Krauss MD and Ron Krauss - Saturated Fat? Red Meat? It Depends. Thomas Dayspring has a nice PDF on his views entitled Understanding The Entire Lipid Profile. The other experts? If you want to get the "full skinny" from Chris Masterjohn PhD, you are better off listening to his three part podcast (or read the transcripts) with Chris Kresser. Forget Gary Taubes and Mark Sisson, neither of whom has ANY special training or demonstrated knowledge of the topic. Instead, you might be interested in the free, informative, two part guest post on Sisson's Mark's Daily Apple blog by Taubes' NuSI partner, Dr. Peter Attia: The Straight Dope on Cholesterol: 10 Things You Need to Know.
Jimmy Moore has assembled an ... eclectic ... group of "experts" with a clear bias among the vast majority, and the opinions of the minority are either absent or even misrepresented by selective quotations. Most appear so blinded by their views on statins that they seem incapable of separating the issues of lipid profiles from statin treatment. Perhaps statins aren't the answer, but adopting a diet that sends your LDL through the roof may still be ill-advised.
So I purchased a copy of this book and am writing this review so that potential customers will have at least one critical pair of eyes on it. The eyes of someone who did not receive a promotional free copy or who might benefit in some ancillary way from leaving a gushing review for Jimmy Moore.
This is not the sort of book to take with you to the doctor and expect to have any sort of constructive conversation to ensue about YOUR health. Most of the MDs have no special training or experience with lipidology and are simply making up their own theories on cholesterol. Before taking any of the sound bites to heart, potential readers would do well to search on The Livin La Vida Low Carb Show and the expert's name to find where Jimmy has published the full interviews behind this book. You can listen to all of them for free.
One major theme of this book is that your doctor has outdated misinformation and is relying on your total cholesterol to put you on deadly statins to make a quick buck for their friends in Big Pharma (the unspoken accusation is that the docs themselves profit from prescribing these drugs). And yet one of these very same "experts" -- The Hamptons Diet author Dr. Pescatore -- is selling a cholesterol lowering supplement on his website! What's in it? Red rice yeast. A statin. Wikipedia has the scoop.
So while many of the MDs and others chime in on how stupid and uninformed your doctor is, they proceed to provide you with unsubstantiated wisdom like (paraphrasing) 'a low carb diet is the best to get your cholesterol where it needs to be' (Pescatore again). But "While he does test for cholesterol levels in patients who request them, 'I never do anything about it. You need to see the whole picture and not focus too much on any one marker,' Dr. Pescatore explained." Odd that he sells a statin-containing cholesterol lowering supplement then.
A second major theme is that fat and saturated fat have no impact on weight or cholesterol levels and carbohydrates do. And yet the aforementioned Pescatore says: "I don't think medical science has any idea why LDL-P would rise above 2,000 or even 3,000 in some people who eat a low-carb [aka a high fat] diet." Yet there are multiple studies showing that saturated fats in the diet DO increase LDL in many people, and "medical science" has a pretty good idea why (search on saturated fats and LDL receptors for the answer).
The author only partially discloses his history of obesity and its relevance to his cholesterol history which is also incomplete. By telling the readers that his cholesterol has always been high he is misleading, because in fact it is higher now than when he weighed 410 lbs. More importantly it was close to normal by mainstream standards after about 10 months of maintenance of his initial 180 lbs weight loss on Atkins. He has been adding a ton of fat to already fatty meals for years now while his weight fluctuated and he hit 300 lbs in 2012. Since May of 2012, Jimmy Moore has been consuming an 80% fat "nutritional ketosis" diet to lose roughly 80 lbs at the one year mark. Aside from other health issues that may be diet related, potential readers should know that he is extremely biased by his attempts to wish his worsening metabolic profile away. If you search on 6 Month Lipid Panel for Jimmy Moore you should find his latest update before this book.
In comments, Thomas Dayspring wrote... "Dr Lipid analysis: Using all the knowledge we possess today, all of the numbers that you are thrilled about have no meaning in the face of a 99th percentile LDL-P. You also should not say an LDL-C of 285 has no meaning. The cholesterol concentrations that often have no meaning are low levels (where an LDL-P is needed to evaluate risk). No one with an LDL-C of 285 with the exception of a Type III dyslipoproteinemia patient have a low apoB or LDL-P. If you have an LDL-C that high, particle testing is not needed. You need to significantly reduce the saturated fat in your diet and see what happens: repeat the NMR in 3 weeks and you will know if your nightmare LDL-P is sat fat related. I'll bet your LDL-P drops. If it does not, you need serious lipid-modulating medication. We have seen this paradoxical horrific rise in LDL-P in some people who are on ketotic diets."
Yet here is the quote Jimmy chose for Dayspring in his chapter on LDL particles (Chapter 9):
"The least accurate way of estimating your atherogenic risk on a standard cholesterol panel would be to look at total cholesterol or LDL cholesterol."
Does this seem like an accurate reflection of Dayspring's full positions on the topic? This chapter should have contained liberal quoting from Dayspring, yet Jimmy Moore claimed on his blog that "I let him make his case in my book."
Dr. Krauss has had this to say about particle number: "But most people certainly in the field of cholesterol and heart disease understand that the number of particles matter more than just how much cholesterol they carry overall. In terms of health, the first order of business is to make sure the total number of particles in a person's blood is maintained in the healthy range, because that's what dictates heart disease risk."
Instead of this information, you get quotes like "If most of your LDL particles are the large, fluffy kind, then you don't have a problem and you have nothing to worry about." This advice comes from Cassie Bjork, who is not even a medical doctor, and has no special training in lipidology. Nevermind that people with familial hypercholesterolemia (a genetic condition characterized by both very high LDL and atherosclerosis) are known for having just that fluffy sort of LDL. And nevermind that both Dayspring would take serious issue with Bjork's advice were he actually given his say ... as it appears would Krauss.
Dr. William Davis (author of Wheat Belly) writes:
"Isn't it funny that people are turning to people like Jimmy Moore for answers to their health problems rather than their own doctors because the doctors have no damn idea what's going on?"
No, it's not funny. It is utterly irresponsible.
If anyone is interested, I have a review post on my blog for this book that shall be updated regularly with new information, including links to reliable sources of information that you CAN share with your doctor: Jimmy Moore's Cholesterol Clarity ~ Ongoing Review and Information on The Carb-Sane Asylum.
Rather than getting information from so-called experts who tell you your doctor is stupid, arm yourself with credible information from credible sources. And if your doctor won't listen, find another one. Internet doctors, and others like Jimmy Moore, will be quick to point out that they bear NO liability for the not-really-medical-advice they dole out. That's just my two cents.
People reading this may have seen my comments left on other reviews. I care deeply that people get accurate information, especially when acting on that information can impact their health. Therefore, I think it is important that folks know:
1. That many of the 5-star reviews were written by people who were provided free advance copies of the book and failed to disclose this per Amazon policy.
2. That many of Jimmy Moore's "world leading experts" are not experts at all.3. That those experts of value in the book are either under-represented or outright misrepresented in this book.
I gave this 2 stars, only because there might be a few folks who discover the names of helpful experts through this book, and might seek further information from them. Otherwise it is a 1 star.
***** ▼▼ Content added 8/28/13 ▼▼
Meet the Experts
These are my cream-of-the-crop experts on the subject of cholesterol.
Jimmy Moore
Cassie Bjork, RD ◊■ Considers Taubes and Moore respected nutrition experts
Philip Blair, MD ◊
Jonny Bowden, PhD
John Briffa, BSc, MB, BS ◊■
Dominic D'Agostino, PhD ■
William Davis, MD ■ Wheat increases chylo and chylo remnants
Thomas Dayspring, MD Understanding the Entire Lipid Profile
David Diamond, PhD ◊
Ron Ehrlich, BDS, FACNEM ◊
Jeffry N. Gerber, MD ◊
David Gillespie (Attorney) ♦
Duane Graveline, MD
Paul Jaminet, PhD ◊■
Malcolm Kendrick, MD Essays on THINCS
Ronald Krauss, MD Extended 2010 interview on Me & My Diabetes , 2012 Saturated Fat? Red Meat? It Depends . . .
Fred Kummerow, PhD Lipid researcher, 98, reports on the causes of heart disease
Dwight C. Lundell, MD ◊■ License suspended
Robert Lustig, MD ◊■
Chris Masterjohn, PhD Podcasts with Kresser Part 1 Part 2 Part 3
Donald Miller, MD ◊
Rakesh "Rocky" Patel, MD ◊
Fred Pescatore, MD ◊ Sells cholesterol lowering supplements
Uffe Ravnskov, MD, PhD
Stephanie Seneff, PhD ◊■ Statins
Cate Shanahan, MD ◊■ The LDL Weight Gain Connection
Ken Sikaris, BSc, MBBS, FRCPA, FAACB, FFSc ■ Sugar and Fat Metabolism video
Patty Siri-Tarino, PhD
Mark Sisson (BA?) ◊■
Gary Taubes, (degrees not listed) ♦■
Key:
♦ = No relevant background
◊ = No particular expertise in the field of lipidology to warrant the term expert
■ = On the record making substantially erroneous claims in the field of human metabolism/physiology such as diminish their credibility as an expert on this topic.
Note: The above key is not "all inclusive" as there are names on that list with whom I am unfamiliar or am not aware of any evidence to warrant the symbol. Don't shoot the messenger here if you take issue with anyone for whom I haven't awarded a symbol -- State your case in comments! If you wish to challenge a designation, I also welcome that discussion in comments.
Also, I'll add links folks might find of interest as I have time (this will not result in popping the feed unless I do a major link dump). I plan on fleshing out some of these as pertains to the content of this book only.
*****
LDL-Connection vs. Statin Treatment
One overall theme that has emerged reading this book is conflating the medical establishment's position on statin treatments with the role of LDL (or other lipoproteins or components thereof) . These two are not two sides of the same coin. Let's look at it this way:
1. There is a pretty good, decades old association between circulating LDL levels and atherosclerosis.
2. There is a connection between diet and lipids though it is generally not as simple as dietary cholesterol and/or saturated fats raising LDL levels. (Though this is pretty simply the case for some).
3. Lowering cholesterol levels through diet and exercise or medications ... here is where the controversy is. What diet is best, is raising HDL necessarily good, are statins treating the symptom but not the cause. These are all valid questions and open for debate. But they do not alter the "facts" of #1 and 2.
For all the focus on diet, I'll say this. MY opinion, to be clear. Any dietary intervention that results in a significant worsening of one's lipid profile is probably ill advised. The first course of action should be to reverse that dietary "experiment".
***** ▼▼ Content added 8/27/13 ▼▼
Meet the Author
Jimmy Moore being interviewed by the Carb-Loaded documentary guys at AHS13 (Aug. 15-17 2013).
*****
Jimmy Moore Misrepresentations
Some of the information here has been discussed before in Hacking Jimmy Moore's Latest Lipid Report. Jimmy Moore lost his 180 lbs in 2004 and maintained the cardio he used to do through much of 2005. He has also increased his carbs to around 100g/day. In October 2005, Jimmy had his lipids tested ... and they were quite normal.
TC = 201 , LDL = 119 , HDL = 71 , Trigs = 57 , VLDL = 11
By March of 2006, things started to go awry and continued through May when he wrote this blog post. A classic quote from Jackie Eberstein (worked as a nurse in Atkins' clinic for many years):
Regarding the hereditary business about my cholesterol being high, Eberstein said my LDL would not have been 119 in October 2005 if it was genetics.
I would tend to agree but it is possible this was a hangover from taking statins as he said his TC got down into the mid 100's on them (pre-Atkins) and elsewhere he stated he stopped taking them in August of 2005 (is it possible it was already climbing?). By May his TC was up to 304 with LDL at 230.
 |
| click to enlarge |
For some reason, Jimmy leaves this information off of the table he shared with his readers during his Nutritional Ketosis experiment, and shares with readers in his book. His timeline begins in 2008. The table from the book is also missing his ApoB results that were included in his 5 year summary on his blog.
It would appear that one tactic to explain away his cholesterol levels is to imply that these have always been an issue, irrespective of his diet and/or weight status. This is not the case, however, which is why including information he has shared from late 2005 and pre-Atkins are important for context. Still, in his podcast interview (for those who would rather not listen, there's a transcript at that link) with Practical Paleo/Balanced Bites Diane Sanfilippo Jimmy said:
I’ve always have extremely high cholesterol levels, and that’s one of the reasons I wanted to write this book. I wanted to find out what was wrong with my numbers for myself...
Not really. And some might be interested in this Twitter exchange that landed in my Inbox:
Before anyone accuses me of persecuting Jimmy Moore, realize that when one lies a lot that is one thing. When one does so in a position where they are disseminating health information and it is relevant, people have a right to know. The above is a lie -- it is only odd that he would continue to do so when he has blogged multiple times about this issue, and is seemingly bragging about negative health markers.
The one thing Jimmy hasn't yet tried is to go back to the way he was eating and exercising circa October 2005.
Before my 180-pound weight loss success in 2004, my doctor prescribed Lipitor for my high cholesterol. At the time, I was morbidly obese and my total cholesterol levels were 230, which he described to me as dangerously high simply because they were above 200.
~ Jimmy Moore in Cholesterol Clarity (KL 938)
Jimmy Moore's cholesterol levels on his current diet are wildly out of the norm, not just slightly high. While 230 is a bit lower than the 275 he reported previously on his blog, if we work off of an average of around 250 -- at 410 lbs drinking over a dozen Cokes a day and eating Little Debbies by the box (his descriptions, many times) -- something very wrong is going on with his CURRENT DIET.
*****
Experts Out of Context
Throughout the book, Jimmy sprinkles "Moments of Clarity" featuring quotes from the various experts. There is a controversy over whether it is particle number or particle size that matters, and it is fair to say that Dr. Thomas Dayspring is a particle number guy. The scientific evidence favors this, and there is not much evidence to support the contention that "large fluffy" cholesterol (or the metabolic milieu underlying it) is benign or, as sometimes claimed, protective. Indeed those with familial hypercholesterolemia (genetic very high LDL) have this LDL size pattern. Jimmy glosses over particle number in the chapter about LDL particles (focusing on size) and clearly downplays this in favor of particle size in the Advanced Health Markers chapter. Something I'll definitely address in the future.
From the beginning of Chapter 9 What’s This LDL Particle Thing? we get a few quotes, among them the one below:
Anyone familiar with Dr. Thomas Dayspring would probably describe him as the "particle number guy". He is someone who works to identify those with normal LDL-C but high particle numbers (also evident in high ApoB) that are at risk. Indeed when Jimmy announced his six month NuttyK lipid profile, Dr. Dayspring had this to say in comments:
Yet the quote above (tan box) is the ONLY contribution from Dayspring in the entire chapter on LDL particles. Indeed much of the chapter is a collection of quotes from the various experts. Definitely more to come on this issue, but know that no bias went into compiling this book!
At least at first glance, Dayspring doesn't get any say on particle number.
#####
#####
Original Introduction to the Post, written 8/27/13
I am not going to mince words here. I consider Victory Belt Publishing to be an utterly irresponsible publishing outfit for publishing a health book, any health book, by Jimmy Moore ... let alone one about cholesterol. Certainly one billed as being helpful for patients to figure out what is going on with their cholesterol levels. As I've stated multiple times, I'm not an adherent of the simplified cholesterol-heart disease hypotheses ... but at this point, neither are most doctors and certainly most scientists working in the field. So if we really want to get to the bottom of this mystery, we need to be looking at what the current scientific evidence is saying. What we don't need is a tome written by someone with a monumental motivation to try to justify to himself that his nightmarish lipid profile is not so nightmarish after all. I would like to see a doctor, especially his co-author Dr. Eric Westman, unequivocally express publicly that Jimmy Moore's lipid profile is nothing to worry about, and that his current diet is not contributing to the problems along with other health issues he downplays.
So I took one for the team, and purchased a Kindle copy.
I know all of these books have the usual disclaimers. They aren't offering medical advice and all that ... but that this one includes 28 "experts" including many that fail to qualify for that title, it is potentially harmful to many people. Thus I will highlight whatever I find pertinent from the book, promotional podcasts, interviews and the like, here in one post. I would add this ... There are some prominent "good names" amongst the list of experts. I think to a one, all would be better served to write their own books on the subject rather than allowing Jimmy Moore to benefit from their reputations and credibility and risk his relaying their information through his biased filter. The first out of context example below is what I'm talking about.
A note to my critics: Doing a review and gathering accurate information, is not stalking or harassing. This is a public service for those who might be inclined to purchase this book based on the 5-star reviews already accumulating on the Amazon webs, glowing reviews on blogs and social media, and a plethora of interviews and podcasts with nary a challenging question. Many of these are by fellow Victory Belt authors and other LLVLC-affiliated (formally or otherwise) people with financial interests of sorts in the game. Please also understand that many of the things I will be sharing are those shared by other concerned individuals who do not have a platform to do so themselves. If anyone has a problem with what is written here (or anywhere on this blog for that matter), you can contact me with your concerns.





Comments
How can you not see how it looks
to post your extremely alarming lipid results, mention that you're
working with a doctor you trust who thinks said results indicate you are
doing tremendous damage to yourself, and, IN THE SAME POST, talk about
how you're writing a book to help people interpret their own lipid
results?
Doesn't listening to Dr. Dayspring (which is a GOOD thing) and
considering what he is saying as arguably valid disqualify you from
writing such a book? How can someone not sure how to interpret their own
results help others?
Now, it is possible you could go through this whole experience, learn
a lot, and then, if you've clearly learned some good information that
helped, end up writing a book about what you've learned. But that's not
what you're doing. You've already signed to do the book and have a
deadline, while you sit there confused by your own results. This is
madness.
LLVLCBlog
Mod
charles grashow
Talk to my publisher. In the
meantime, I'm interviewing the best and brightest people who know their
stuff in this arena (Dr. Dayspring included, who I am visiting in VA
next month). The reality is nobody knows what the importance of LDL-P
and/or Apo B are for people on a ketogenic diet. Maybe I can help solve
this mystery for the many others out there who are in this same
situation that I am. I appreciate your concerns and your feedback,
Charles.
charles grashow
Jimmy - you said "My blood work
from October 2005 showed my lipid profile as nearly ideal with HDL at
71, triglycerides at 57, VLDL at 11, LDL at 119, and total cholesterol
at an acceptable 201. This was what my numbers looked like after livin’
la vida low-carb for about 22 months and I was proud to see them doing
so well."
What have you changed since then and why don't you go back to what you were doing then??
LLVLCBlog
Mod
charles grashow
What was working then doesn't work for me now 7 yeas later. Thus, I adjust.
Charles grashow
Why did you change what was working then and why do you think it won't work now??
LLVLCBlog
Mod
charles grashow
Because what was working then stopped working or me. You adjust and make appropriate changes as I've done.
Let the Moore acolytes whine, but if what you say has merit, then it has merit. If what Moore says has merit, it has merit.
So far the book seems to mostly be a collection of quotes from interviews, many of which are not with experts after all.
Think what anyone will of me and my credentials, etc. I would not agree to be interviewed as an expert for such a book because I am not one! Neither is Mark Sisson, Cassie Bjork, Cate Shanahan, Paul Jaminet or Gary Taubes (to name a few).
What the HDL does what any of the above *think* have to do with anything?
I'm just going to put this here in this comment: http://www.lipidcenter.com/pdf/Understanding_the_Entire_Lipid_Profile.pdf
SUMMARY: To read a lipid profile properly and effectively:
1) Look at the TG: If > 500 treatment is needed and the TG takes precedence over all other lipid concentrations. If TG are less than 500, go to step (2)
2) Look at the LDL-C, because if it is above 190 mg/dL, drug therapy is indicated no matter what else you find. At lesser levels it depends on the risk of the patient whether drug treatment is indicated.
3) Look at the HDL-C: concern if < 40 male or 50 woman
4) Calculate the TC/HDL-C ratio: Concern if > 4.0 Some advocate LDL-C/HDL-C ratio, but I do not since LDL-C is a calculated value
5) Calculate the non HDL-C (TC minus HDL-C). NCEP says to do this only if TG are > 200, but in reality this calculation is always equal to or better than LDL-C (less valuable if TG >500)
6) Calculate the TG/HDL-C ratio
7) If apoB/apoA-I ratio is so predictive (and it is): you can estimate it by looking at TC/HDL-C or Non HDL-C/HDL-C
All should know that the NCEP goal for Non HDL-C is 30 mg/dL higher than whatever the LDLC goal is for a given patient. Thus if your LDL-C goal is 70 (very high risk patient), the Non HDL-C goal would be 70 + 30 or 100 mg/dL. In a primary prevention setting where NCEP calls for an LDL-C of 130, the non HDL-C goal is 160. I agree with the AHA Women's Guidelines: all adults should have a non HDL-C < 130 mg/dL.
_________________________________-
Now I'm not saying Dayspring is the final word be all and end all, but I have yet to come across anything (that is a yet) indicating these are his positions on the matter.
I put comments on Seib and Fragoso's reviews because they are VB authors and Amazon rules state you are supposed to stipulate if you received a free copy in exchange for a review, etc.
Mark Sisson is a leading authority in the low-carb movement, as well as an expert in evolution-based health, fitness, and nutrition. A noted researcher, author, and lecturer, he has dedicated his personal and professional life to offering sustainable solutions for health, wellness, and weight loss. He is the author of the Amazon best-seller The Primal Blueprint. He is also the founder and CEO of Primal Nutrition, Inc., a provider of health education materials and lifestyle-enhancing nutritional supplements. Sisson attended Williams College, where he received a BA degree with a major in biology. As an elite endurance athlete, he finished fifth in the 1980 USA National Marathon Championships (2:18:01) and fourth in the 1982 Hawaii Ironman Triathlon.
He was an arthritis riddled grain eater back when he was an endurance athlete. His cholesterol must have been hideous ;-)
Primal fuel, the ultimate lifestyle-enhancing nutritional supplement!
If so, it's really odd that she is running a "special offer" inducement to buy Jimmy's book.
Now ... I wouldn't have to "rip everyone a new asshole" if they weren't so deceitful. Wouldn't it just be preferable if folks stuck to facts and stopped making shit up to sell stuff?
Have a nice day!
Clearly Dayspring has fallen in with Taubes on the diet solution more recently, but that does not change his opinions on cholesterol based on the scientific evidence of which he seems well familiar and comprehensive in evaluating.
Here is the link http://www.plantpositive.com/17-thomas-dayspring-lipidologi/ which contains the video and a transcript, and here is the video: http://www.youtube.com/watch?v=uSzByKafWKM#t=102
I didn't listen to Dayspring's podcasts with Jimmy but it would be interesting to see how much he stood up for his positions.
I realize Jimmy would like to wave the magical NK fairy wand at his lipid panel and declare it irrelevant because of his ketones, but one could just as easily make the case for the low triglycerides being deceptively so (more fat stored in the liver than exported). Indeed I think that case is likely stronger when you get to pathological lipids like his.
So the question remains, are you an internet troll... or are you an expert?
would that be the drug that causes ulcerative colitis, the drug that causes myositis, the drug that causes neural degeneration, or just one that increases cancer and diabetes risk?
You would have to really hate LDL, but is that hatred justified?
Here's a novel idea - consider cholesterol (why serum? Why not cellular? Oh that's right, we only have a test for serum) in the context of diet, pollution, and other stressors etc.
If you are eating crap that will kill you and not exercising and breathing air pollution, your cholesterol scores are likely to be indicative of high risk. Whatever they are.
I'll have to think hard to find a person less healthy and less fit than Mr. Moore. And even more so there is probably nobody in this "industry" giving worse and more damaging "health"-advice than Mr. Moore.
http://www.reuters.com/article/2012/11/07/us-statins-cancer-idUSBRE8A62H020121107
To make it easy on readers, the title on this 06/13/2013 overview will suffice: "Statins and Cancer: More Questions Than Answers"
http://www.huffingtonpost.com/dr-paul-j-rosch/statins-cancer_b_3436148.html
The author is obviously no fan of statins, either. Me, neither.
http://www.amazon.com/review/R3VQ2DF5AM8N4R/ref=cm_cr_pr_cmt?ie=UTF8&ASIN=1936608383&linkCode=&nodeID=&tag=#wasThisHelpful
However, and this is the important part, when the authors adjusted for the number of LDL particles (in yellow), the same phenomenon was not observed. Now an increase in LDL particle size by 1 standard deviation was associated with an ADDITIONAL 14.5 microns of atherosclerosis, albeit of barely any significance (p=0.05).
Let me repeat this point: Once you account for LDL-P, the relationship of atherosclerosis to particle size is abolished
out this post from Anthony Colpo (assume his opinion will meet your standards considering
he's very fit). "… why, if they know so much about fat loss, are Taubes
and Lustig in such appalling shape? These individuals openly ridicule both the
“calories in/calories out” paradigm of weight loss and those of us who sensibly
acknowledge it, so why are they the ones sporting such prodigious waistlines?"
http://anthonycolpo.com/luke-sissyfag-gary-taubes-robert-lustig-the-problem-with-journalists/ Please enlighten me on why it matters what you look like again? :)
He would need a baseline scan to show evidence of regression, or halt of advance, or perhaps slowdown of advance. Then it gets tricky for him, because he apparently did have a good scan years ago. But that scan followed his overeating on SAD for decades, true? So he can't claim that a good scan now resulted only or primarily from LC.
So he needs some case study that uses repeat scans of somebody that says that they actually achieved plaque regression on some sort of LC diet. But then there is the possible counterclaim that such a subject is somehow oddly different. You wouldn't expect that a smoker who lived past 100 should write a book claiming that everybody should smoke. That means, as always, that we should rely on data from large numbers of subjects, and that data indicates that high cholesterol numbers are dangerous. You can't use one or two anecdotes to try and overturn the dreaded conventional wisdom... unless you are appealing to the easily influenced, which is what they are doing :)
However, the anti-inflamation idea has validity on its own, as apart from how it might be used or misused here. Then they have to explain away how the powerful inflammation lowering effects of statins aren't lifesavers.
Chris Kresser:
Theoretically not as big of a risk factor for heart disease. And then pattern B would be that you have a bunch of small dense, LDL particles and the idea was that these are were more harmful, more likely to damage the endothelium and initiate the whole process of atherosclerosis. But more recent research has shown that there are a couple of problems with that theory. There's no doubt that smaller dense of LDL particles can be a sign of
something gone wrong. But in studies that control for LDL particle number, they found that the association between small dense LDL and heart disease disappeared. So in other words, if they did a study and it only measured small dense LDL protocol number and heart disease, they found a correlation. But if they also measured just a Number of all LDL particles, then the predicted value of small dense LDL particles disappeared.
So what that suggest, of course, is that it's the total number of LDL particles regardless of whether they're large and fluffy or small and dense. That's the most important factor. And getting back to your earlier question, how do we measure that? The gold standard for measuring that is a test called the NMR, nuclear magnetic resonance test. And it's offered by a lab called Lipid Science. It's the only lab that's FDA approved for determining LDL particle number, which is often referred to as LDL particle concentration. So you take that test and the result comes back and it tells you the number of LDL particles that you have. And that turns out to be the main driving factor in atherosclerosis because it's a gradient driven process, which means that the more particles that you have floating around in your bloodstream, the more likely it is that some of them are going to migrate into the endothelium, damage it and start this process of platforming.
Rob Wolf
So it's just kind of a statistical gig, like, even though small dense LDL maybe more reactive even large puffy LDL particles, at some point, if we have enough of them, just statistically, we're going to call some damage in the endothelium, get some inflammatory response and then...
Chris Kresser:
Right. And that's one of the actually, one of the actually, was one of big holes in the theory of that large buoyant LDL was not a problem, is that people with the condition called familial hypercholesterolemia, which is a genetic problem that we'll probably talk about in a few minutes here where people produce they have a much higher number of LDL particles than someone without that condition. Well, people with this condition have a whole bunch of particles and then mostly large buoyant LDL particles. But they have a three times greater risk of heart disease than someone without that. So even though all of their LDL particles are large and fluffy, they're still having, you know, they have 300 percent higher risk of heart disease?
– Dr. Jeffry Gerber
Jimmy Moore - from his new book
– Dr. Chris Masterjohn
> a longer list of testimonials and people they have helped than you
So obiously you'll take Sylvia Browne's testimonials list and pay her
while ignoring my advice to ignore her
How about Fred Hahn & Mike Eades - are they throwing in some bromance-marketing in there?
Jimmy Moore - TC 310, HDL 66 - ratio 4.70. Should he be concerned??
ultra-high fat VLC diet. My
LDL was 1.8 (60). HDL was 5.9 (228). This is the polar opposite to Jimmy Moore. [The probable explanation was my extremly high actvity levels, lowish BMI (~23-24) and fasting 20hrs/day.]
Mathias Rath is killing people with his pseudo-therapies and his ridiculous hypothesis won't help anyone to avoid heart disease.
Standard Lipid Panel
Total Cholesterol Mostly irrelevant, but women should be 250 mg/dL or below and men should be 220 mg/dL or below
LDL-C 130 mg/dL or below, but higher levels are not necessarily relevant to your heart
health risk.
HDL-C Above 50mg/dL is good, but 70 mg/dL or higher is best
VLDL-C Between 10 and 14 mg/dL
Triglycerides 100 mg/dL or below, but under 70mg/dL is best
Non-HDLCholesterol No evidence of an optimal level
– Dr. Fred Pescatore
– Gary Taubes
But a casual look at Jimmy's figures shows that, e.g., LDL-C goes up and down according to bodyweight.
250
201
119
252
172
304
230
332
250
326
246
298
228
351
278
386
290
342
257
359
285
410,250
201,119
252,172
304,230
332,250
326,246
298,228
351,278
386,290
342,257
359,285
His current weight is unknown. I'm going to put it at 245 as he mentioned gaining 15 lbs on FB (blamed on teeth pulling saga) and he looks heavier than he did at PFX.
It shows the linear relationship to weight. Once points are added for the extreme diet period, I wonder if the line gets broken. I.e., low weight but increasing LDL-C.
What is the worst LDL?
The simplest way to describe it is as large and small. These are cholesterol containing balls of fat that come in different sizes. And the larger forms of LDL carry cholesterol but they don’t seem to do as much damage to the arteries as the smaller LDL particle.
---------------------------------------------------------------
As much damage is a far cry from the general tone in the book that large LDL is benign.
Glad that was of some help. Seneff is the sulfur one; I can't guess the association here offhand. Ravnskov is the one who supposedly demolished Keyes' seven country statistical association by adding more countries. Finally, that perky Paleo woman wrote a long blog about how the association was indeed significant. But she ended with "association is not causation" and so got the usual cheering.
Okay, I found it by searching cheeseburger. http://www.meandmydiabetes.com/2012/04/17/ron-krauss-saturated-fat-red-meat-it-depends/
RON KRAUSS
Both numbers can be helpful. But most people certainly in the field of
cholesterol and heart disease understand that the number of particles
matter more than just how much cholesterol they carry overall. In terms
of health, the first order of business is to make sure the total number
of particles in a person’s blood is maintained in the healthy range,
because that’s what dictates heart disease risk. Beyond that, when the
total amount of cholesterol is unusually high, you’ll almost always find
that the total number of LDL particles is high. And looking even
deeper, when the total number of LDL particles is higher than normal, I
and many of my colleagues would argue that the biggest concern is
warranted when the number of smaller particles is high, not the larger
ones.
RON KRAUSS
To begin with, keep in mind, this was a very high beef diet. People
were eating beef breakfast lunch and dinner. So this is really way
outside of what we would ever consider to be a usual health practice.
Maybe some people do it. But not many. We were really interested in
the metabolic impact of this diet. To get as many clues as possible, we
fed people in either the context of lean beef alone, or with extra
saturated fat, mostly from diary products. Again, that’s because most
of the saturated fat we get in our diet comes from dairy products.
There’s some saturated fat in beef, but more in dairy fat. To make
things as clear-cut as possible, in this study, we fed the same beef
product to two groups. Lean beef, low in fat, without any added
saturated fat. For one group, we added lots of dairy fat, to increase
saturated fat. For the other group, we kept saturated fat low, but kept
total fat basically the same by using an unsaturated fat–basically
olive oil. So between the two groups, let’s say the difference was the
equivalent of a cheeseburger versus a lean hamburger dressed with olive
oil. That sort of describes, in a nutshell the kind of differences we
were looking for. When we did blood work on the groups, the group who
ate lots of beef with low saturated fat, meaning the olive oil, didn’t
seem to have any adverse effects.
Meaning the blood work you did on that group didn’t
reveal an increase in the LDL particles and other biomarkers that
indicated heart disease risk.
RON KRAUSS
We didn’t see any adverse effect if we just fed a high beef diet in the absence of saturated fat.
RON KRAUSS
The punchline is that we expected that because these diets have low
carbohydrate, when we fed the high saturated fat level along with the
red meat, we would see a pretty benign metabolic risk profile. Just as
we did with low saturated fat and red meat.
But that’s not what happened!
RON KRAUSS
This is one of the surprises that keep life interesting for us for us as
researchers and also for the world out there who happens to be looking
over our shoulder. In this case, the surprise was that the combination
of the high beef diet and the high saturated fat diet caused very
serious increases in all of the cholesterol related risk factors we had
been measuring, including total particle numbers, small LDL, total LDL
cholesterol, inflammation, whatever we looked at, we saw an adverse
effect.
Everything went wrong.
RON KRAUSS
This was in contrast with our earlier studies where the same amount of
saturated fat and very similar carbohydrate intake but a diet not loaded
up with red meat, had no adverse effect even if it had lots of
saturated fat in it.
SO - beef + saturated fat = trouble?? WWJS (What Would Jimmy Say)
Do you know of a good rundown / synopsis of the critique from a couple of years ago that Statins don't improve all cause mortality? Has there been a denouement or is this issue a work in progress?
I got interested and then life "took a turn" and it dropped off my radar, and now the searches produce a lot of popular-audience-noise
Bunch of links would be fine, preferably to balanced skeptical analyses.
Yet in some of these isolated sub-cultures cherry picking rules the day. The opposition's erased or minimized.
I wonder if It only works with audiences that want the cherry picked certainty/reinforcement.
Sorry, I don't have links on the topic you mention. My main interest in statins is in seeing how easily they now produce plaque regression. The SATURN trial had two drugs going head to head, so establishing quick and easy regression is taken for granted now. Back in the 1990s, Ornish got only a little bit in regression in only some subjects, with a lot of difficult lifestyle modifications.
Effect of lipid-lowering therapy with atorvastatin on atherosclerotic aortic plaques detected by noninvasive magnetic resonance imaging
Conclusions
One-year 20-mg atorvastatin treatment induced regression of
thoracic aortic plaques with marked LDL cholesterol reduction, whereas it resulted in only retardation of plaque progression in abdominal aorta. Thoracic and abdominal aortic plaques may have different susceptibilities to lipid lowering.
http://content.onlinejacc.org/article.aspx?articleid=1138009
Simvastatin Attenuates Plaque InflammationEvaluation by Fluorodeoxyglucose Positron Emission Tomography
Conclusions
18F-fluorodeoxyglucose PET visualized inflammation of atherosclerotic plaques and that simvastatin attenuated it. The anti-inflammatory effect of simvastatin on the plaques may be one of the pleiotropic effects independent of LDL-C–lowering effects.
http://www.ccjm.org/site/misc/Oct06_Sipahi.pdfCoronary atherosclerosis can regress with very intensive statin therapy
He did a Jimmy talk about a year ago. http://www.lowcarbconversations.com/970/62-kaleigh-laventure-dr-rakesh-patel/
It is downright compelling when he describes how he had two bumps show up on a CIMT sonogram, then he went Paleo and on his next scan the bumps were gone. He say the plaque regression was because the HFLC is so very low on inflammation, no evil carbs. That's got wow factor, but... there is something that he leaves out. A really big something, in fact. Suspenseful? I bet the unspoken counter is not in this book, either.
If somebody listens to it soon maybe they can post the timestamp where he describes the sonograms. It's probably nearer to the end than to the beginning.
LDL-P is not as predictive as carotid total plaque area.
Awesome blog.. except for all the sniping, but that seems to be par for the course on any blog..
They have a amazing atmosphere with the amazing decor.
It is hideaway and intimate, usually it is not packed crazy.
You feel like you are in the cold, stylish and comfortable living room with comfortable sofas and chairs.
They also have a small patio outside so that you can take advantage of the warm day in SF. Their private dining space suitable for 10-15 people looks cold as well. Their service is friendly and helpful.
I have been debating whether I ought to share my favourite spots here, but sharing is caring...
I am liking coming here before dinner for my glass of wine accompanied with their cheese plate.
Great place for a date or for a small group girls night to enjoy the intimate feel.
Highly recommended for cold wine lovers. http://www.coffeepurecleanseus.org/
Watching Jimmy Moore talking for a few minutes should be enough to make every halfway sane person run away screaming. The fact he is considered a reliable source of "information" by many is very telling.
1) People with FH have up to 13-fold increased risk of CHD (increased RR for all-cause mortality unknown), according to http://www.ncbi.nlm.nih.gov/pubmed/23956253
2) Statins decrease the RR for CHD for some types of FH (decrease in RR for all-cause mortality unknown), according to http://www.ncbi.nlm.nih.gov/pubmed/20595220
Therefore, people with FH probably benefit from chol reduction. However...
According to MRFIT, people with TC up to 6.7mmol/L (259mg/dL) have a modest increase in all-cause mortality from the minimum, so needn't be medicated. Sadly, money seems to trump everything else.
the number of LDL particles that is physiological normal doesn't greatly
increase the risk of plaque build up. Numerous animal studies for all
sorts of different species show the same thing. You jack their LDL
cholesterol up and keep it up for a period of time and they develop
heart disease.It seems to be the game some low carbers are
willing to play with. No matter how nightmarish the markers are they
have some kind of illogical faith that the magical powers of ketosis and
butter will protect them.
Now I'm not saying you were doing that, just that most who see the LDL go wonky usually are taking the HF to way excess. Even Atkins acknowledged that his diet wasn't good for some.
Early on in this blog I blogged on a study showing CRP going up: http://carbsanity.blogspot.com/2010/02/low-carbohydrate-high-fat-diet.html
As I said above (or below), Jimmy missed a golden opportunity to really pick these two's brains. That wasn't the purpose of this book. :(
It is around the 35 minute mark where he discusses improvements in his CIMT but exploding LDL particle number consistently around 2500 and up over 3000.
Coincidentally he responded to a tweet of mine about Trig/HDL ratio yesterday. I'm going to see if I can't chat with him one-on-one!
Alterations in cholesterol absorption/synthesis markers characterize Framingham Offspring Study participants with CHD
In conclusion, present results indicate that alterations in cholesterol
homeostasis, namely high cholesterol absorption and low cholesterol
synthesis, are associated with increased CVD risk in a subset of men and women with similar plasma LDL-cholesterol concentrations. Additionally, the cholesterol homeostasis markers appear to be better predictors of disease than traditional lipid risk factors in this study population.
http://jn.nutrition.org/content/141/10/1791.full
Cholesterol-Absorber Status Modifies the LDL Cholesterol–Lowering Effect of a Mediterranean-Type Diet in Adults with ModerateCardiovascular Risk Factors
Cholesterol synthesis/absorption status was not markedly altered
by diet, but the decrease in plasma LDL-C due to the Mediterranean-type diet occurred only in low absorbers of cholesterol. This should be considered during further dietary interventions.
The present study provided 2 main findings. First, we showed
that the cholesterol absorption status or the synthesis/absorption status based on serum surrogate markers, as observed with an habitual WD, remained unchanged after 3 mo of consuming the LFCMD. Second, cholesterol absorption status in combination with dietary regimen altered the plasma concentrations of cholesterol and LDL-C in the 2 sexes.
In conclusion, the present study of 125 men and women at
moderate cardiovascular risk provides 2 important pieces of information. First, the synthesis/absorption balance for cholesterol, the key for cholesterol homeostasis, is likely an intrinsic trait of the participants that is not noticeably altered by changing the diet. This applies to both men and women; thus, there is no apparent sex specificity. Second, we showed that the
cholesterol absorption status of both men and women is a clear determinant of responsiveness to a healthy dietary challenge by predicting a significant lowering of LDL-C in participants with a low-cholesterol absorption status. If this observation is confirmed by other studies, it may be possible to measure the serum surrogate markers in men and women at CVD risk to determine the cholesterol absorption status and thus to predict whether a given individual may be able to lower LDL-C with dietary modification. Finally, the observed correlations between insulinemia or insulin resistance status (HOMA-IR) and cholesterol synthesis:absorption ratios (Supplemental Table 1) were stronger in women than men.
I am not arguing that Atkins is not dangerous for some. To the contrary. I have pointed these dangers out here on this blog multiple times. However in the short term for most I don't think it is bad for weight loss -- indeed for whatever reason, the more obese and sedentary a person is, the better the SHORT term outcome. My personal opinion is that LC is good for 6 months to a year and once weight loss has been achieved, should be gradually phased out. If a person can't eat a small potato without a glucose spike they aren't healthy.
Glucose is not an aggressive cause of inflammation. That's LC pseudoscience.
http://circ.ahajournals.org/content/116/16/1832.full
It "doesn't make sense" to have LDL-C higher than ~40-80 mg/dl either if you realize that's what all primates and other mammals have.
I could not agree more with you that the diet is great until the weight is lost and then should be phased out. Pretty much what I did, although I lost 10-15 lbs more post-Atkins. The Atkins diet taught me to stop eating junk food - unfortunately, it didn't tell me to stop eating fast food (I did that later). I'm now vegetarian - not for health reasons, mind you, although it works best for my lipids - mainly for ethical and spiritual reasons. I try to keep my carb burden down - hard to do as a vegan but I definitely had metabolic syndrome pre-Atkins.
Thomas Dayspring
@Drlipid
28 Feb
@dwightlundell His glu was ~120 What you really mean is that it was his insulin resistance driving many vascualr biomarkers inc apo B
Ketogenic diets are known to produce kidney stones in generally unsusceptible populations. I don't suppose any inflammation accompanies that?
> Glucose will always be present and will always cause damage.
so will bacteria, allergens, viruses, environmental irritants, excess nutrients, white blood cells dying and spilling ...
And glucose is so bad the body will catabolize heart tissue to make some (thanks to Kurt Harris for introducing me to this)
> no such thing as 0% A1C
and if such a thing were possible how would that be a good thing? (I typed this before Evelyn replied above)
> Glucose will always be present and will always cause damage.
so how much damage does it cause in the Kitavans (who also smoke heavily)
Mr. Russert’s cholesterol was not high, and medicine controlled his high blood pressure pretty well, Dr. Newman said. But, he added, Mr. Russert was “significantly overweight.” He also had a dangerous combination of other risk factors: high triglycerides, a type of fat in the blood, and a low level of HDL, the “good cholesterol” that can help the body get rid of the bad cholesterol that can damage arteries.
In an interview, Dr. Newman and Mr. Russert’s cardiologist, Dr. George Bren, said the autopsy found significant blockages in several coronary arteries, which feed blood to the heart muscle.
In Mr. Russert’s case, the heart attack was caused by a plaque
rupture in a branch of the left anterior descending coronary artery. The heart attack led to an abnormal heart rhythm that stopped his heart from pumping blood effectively and caused his death.
“What is surprising,” Dr. Newman said, “is that the severity of the anatomical findings would not be predicted from his clinical situation, the absence of symptoms and his performing at a very high level of exercise.”
In 1998, Mr. Russert had a calcium score of 210 on a CT scan
of the coronary arteries, a test that indicates blockages. The result
called for “an intensive cardioprotective regimen,” Dr. Newman said. That level can indicate a moderate to high risk of a heart attack.
Dr. Newman and Dr. Bren said that in the past year, Mr. Russert’s blood pressure had risen a bit, and that they had changed his drug regimen to lower it. His heart muscle had also thickened. Some cardiologists say a thickened or enlarged heart can indicate severe heart disease and should prompt more tests, like an angiogram, to look for artery blockages. But those tests are invasive, and Mr. Russert’s doctors did not think he needed them.
Had the tests been done and the true extent of blockages revealed, Dr. Newman said, Mr. Russert would probably have been advised to have bypass surgery. Dr. Bren differed, saying it was not clear that there was enough disease to prompt a recommendation for surgery.
http://www.nytimes.com/2008/06/24/health/24hear.html
On the negative side, Mr. Russert had low HDL, the protective cholesterol, and high triglycerides. He was quite overweight; a waist more than 40 inches in men increases heart risk. A CT scan
of his coronary arteries in 1998 gave a calcium score of 210,
indicating artery disease — healthy arteries do not have calcium
deposits — and a moderate to high risk of a heart attack. An
echocardiogram in April found that the main heart pumping chamber had thickened, his ability to exercise had decreased slightly, and his blood pressure had increased a bit. Dr. Newman and his cardiologist, Dr. George Bren, changed his blood pressure medicines, and the pressure lowered to 120/80, Dr. Newman said.
Here is what Jimmy says in the book:
Tim Russert’s “Perfect” Cholesterol Numbers
Tim Russert had his first heart attack as he was preparing for the show he anchored, Meet the Press, and it instantly killed him. He was just fifty-eight. Ironically, Russert had been doing everything that his doctors advised him to do to prevent a heart attack: He was taking a statin drug, another medication to lower his blood pressure, and faithfully riding an exercise bike everyday. Here’s the most shocking part of this story: his total cholesterol was just 105! And yet his very first heart attack was fatal.
...
According to Russert’s doctor, he didn’t have type 2 diabetes, nor did he have any blood sugar issues. His A1c was in the normal range and his cholesterol was considered very healthy. For all intents and purposes—and according to the modern medical convention of looking at health on paper—he was the epitome of perfect health. We now know, posthumously, that Russert had coronary artery disease and was being treated for it, but his doctor apparently didn’t know how severe it was. But even if he had known, the likely course of treatment would have been a higher statin dose, a diet even lower in fat, and maybe some more exercise. In all likelihood, none of those supposedly prudent strategies would have prevented
...
Most doctors would look at Russert’s total cholesterol number and see nothing but health. They would extol the virtues of the statin drugs that artificially put his cholesterol numbers within the so-called “acceptable” range. But what good did it do him in the end? People were perplexed and confused by his death, but no one seemed terribly angry about it. I find that response to this incredibly strange. People should have been outraged—but they weren’t. Russert’s health was not only made worse by modern medicine, but his death was almost entirely preventable!
....
Then there's Dayspring:
“When we were a non–insulin resistant country, all we had to deal with were genetic lipid disorders. We had high cholesterol levels that correlated nicely with ApoB or LDL-P. But when people started eating too many carbs, our insulin resistance genes suddenly began expressing themselves. That led us down a path where triglyceride molecules started to invade the LDLs and HDLs, thereby displacing the cholesterol molecules. As a result, cholesterol was looking great, but then you have a sudden death like Tim Russert’s. His high triglycerides resulted in low total cholesterol and LDL-C and very high ApoB and LDL-P, paradoxically raising cardiovascular risk by dropping LDL-C. Unfortunately, he also had a lot of atherosclerotic plaque that ruptured, which led to a thrombus, coronary artery occlusion, and myocardial infarction. If clinicians working with such patients would pay a little more attention to non-HDL cholesterol, they would not be so reassuring to those patients that their great LDL cholesterol levels are somehow protecting them against a fatal heart attack. Tim Russert was like so many insulin-resistant or type 2 diabetic patients: a dead man walking.”
Blood sugar issues are generally downstream of the lipid disturbances folks.
I personally might assume that plaque reduction could be a bad thing because it's plaque mobility or tendency to rupture that's the worst thing, and plaque reduction could increase that tendency.
Thoughts? Links?
Is there a U-shaped curve of A1c versus mortality?
http://www.leicestershirediabetes.org.uk/uploads/121/documents/The%20Lancet%20Survival%20as%20a%20function%20of%20HbA1c%20a%20cohort%20study.pdf
Survival as a function of HbA(1c) in people with type 2 diabetes: a retrospective cohort study.
Abstract
BACKGROUND:
Results of intervention studies in patients with type 2 diabetes have led to concerns about the safety of aiming for normal blood glucose concentrations. We assessed survival as a function of HbA(1c) in people with type 2 diabetes.
METHODS:
Two cohorts of patients aged 50 years and older with type 2 diabetes were generated from the UK General Practice Research Database from November 1986 to November 2008. We identified 27 965 patients whose treatment had been intensified from
oral monotherapy to combination therapy with oral blood-glucose lowering agents, and 20 005 who had changed to regimens that included insulin. Those with diabetes secondary to other causes were excluded. All-cause mortality was the primary outcome. Age, sex, smoking status, cholesterol, cardiovascular risk, and general morbidity were identified as important confounding factors, and Cox survival models were adjusted for these factors accordingly.
FINDINGS:
For combined cohorts, compared with the glycated haemoglobin (HbA(1c)) decile with the lowest hazard (median HbA(1c) 7.5%, IQR 7.5-7.6%), the adjusted hazard ratio (HR) of all-cause mortality in the lowest HbA(1c) decile (6.4%, 6.1-6.6) was 1.52 (95% CI 1.32-1.76), and in the highest HbA(1c) decile (median 10.5%, IQR 10.1-11.2%) was 1.79 (95% CI 1.56-2.06). Results showed a general U-shaped association, with the lowest HR at an
HbA(1c) of about 7.5%. HR for all-cause mortality in people given
insulin-based regimens (2834 deaths) versus those given combination oral agents (2035) was 1.49 (95% CI 1.39-1.59).
INTERPRETATION:
Low and high mean HbA(1c) values were associated with increased all-cause mortality and cardiac events. If confirmed, diabetes guidelines might need revision to include a minimum HbA(1c) value.
I did have kidney stones back in the 1980s but that was towards the end of my nearly 20 years as a low fat high carb vegetarian. My current nearly 10 years as VLC/ketogenic does not appear to be causing any kidney issues, and all my inflammation markers, CRP especially, as of last week show very low risk of CVD. But then my family have no history of heart disease and they died at ages 92 and 97 through non heart related issues.
So how much does genetics play into this? Lipoprotein(a), and APO E for example, or something else. My TC and LDL-C levels would be considered high yet my HDL is high and trigs are low. I am interested in Jimmy's book and related discussion because I appear to be in a similar position to Jimmy. I do not hold an entrenched position but VLC/keto appears the most healthy for me right now. I'm looking for either confirmation or rebuttal and I will adjust accordingly.
Right now though the current official guidelines on cholesterol and the use of statins appear to be entirely irrelevant to my ketogenic lifestyle as Jimmy also appears to conclude. But if true then why?
But regarding glucose - it seems clear there are folks and even cultures that can tolerate and thrive on high levels of carbs and others that do less well. The determining factors appear large differences in hormone and enzyme expressions and other genetic factors, as well as environment and geography - e.g. those acclimatized to the tropics for the past 500K years (high plant based) will differ from those acclimatized and adapted to the arctic, e.g. Inuit types, with near to zero vegetation.
It seems reasonable to assume that with so much variation it makes no sense to say there is a single optimal dietary regimen that fits everyone. And similarly the cholesterol level guidelines should not be applied to everyone without regard to a large host of other individual and dietary factors.
SO - wouldn't that be a reason to be concerned with a high LDL-P (like Jimmy Moore's >2700)??
In a similar way there are no animals in the wild that need to understand or count calories to stay healthy and lean even when given an environment of plenty.
We appear to have artificially corrupted our own food supply that causes severe metabolic imbalances for the majority of people. We should neither need to be aware of calories or cholesterol levels to remain naturally healthy and lean.
But "we" actually DON'T maintain tight levels of LDL-C! Free living "primitive people" living like traditional hunter-gatherers regularly have levels of TC well below 150mg/dl. As you say it's "our" sedentary lifestyle and general overconsumption of food that makes these levels deteriorate. And guess what, practically everybody whos is willing and able to implement drastic(!) changes in lifestyle and nutrition is able to reach these levels.
But that would be fine for those starting out and are young. Our biggest problem now are those who have damaged themselves from years of abuse with junk foods etc and are now metabolically damaged. In particularly the obese and those pre-diabetic or actually diabetic, insulin resistant, etc. Trying to lose weight for example is proving extraordinarily difficult - and eating less and moving more, clearly and simply does not work for the vast majority.
As I commented elsewhere, Tim Russerts inflammatory markers were low too.
It seems like this book is the perfect one for you as you want to be reassured that indeed all bets are out the window because of the magic of insulin. I hope that's true. Doubt it though.
I think anyone whose total cholesterol goes over 300 on Atkins is headed for trouble (that was my case - my total went to 308, and my LDL was nearly that high too). My inflammatory markers virtually disappeared and my A1c plummeted to 0.047. Homocysteine went from 9.5 (measured years before Atkins) to 17.6 on Atkins (methionine loading). Trigs plummeted, HDL doubled. It is almost the perfect picture of familial hypercholesterolemia (het), or cholesterol hyperabsorber syndrome, or the response of my liver to a daily saturated fat load.
I am now completely vegan. I haven't done any bloodwork in about a year because I no longer care all that much about it (but when I did last check it, the lipids had normalized off statin). I do track my weight (~127-128 lbs) and BP, but not all that regularly.
My whole point is that Atkins or LCHF or ketogenic diet can seriously harm certain individuals, particularly if they are not monitoring their bloodwork. I actually had a VAP done to confirm what species of LDL and HDL I had. I think your point that Atkins is a great diet for weight loss and then should be gradually phased out is a wonderful one. Hopefully even vulnerable people can tolerate 6-12 months of severe hypercholesterolemia, and then switch to something more sensible. Perhaps people with my ethnicity were not meant to be consume that much cholesterol ester and saturated fat. Pretty sure my current diet is not as carcinogenic either...
Why are you not very concerned about those test results? Over HALF of your particles are small!
I believe I am super sensitive to carbs, although alcohol is not carb and I do not understand how that change would have affected my metrics.
I take no meds, weight is 185, morning FBG hovers just over 100. Was pre-diabetic back in 2004 at fbg=120. Doctor suggested reducing carbs.
I am debating what to try next. Just want to change one thing only.
I don't know whether to be concerned or not. Inflammation markers say I have low risk so I suspect these NMR metrics may not be meaningful. I think I will get a calcium CT scan next.
Big Pharma didn't fund this research, the authors merely disclosed past honoraria from some sources. Think what you want about the pharmaceutical industry ... without them we don't know half of what we know today.
The book has significant value from the perspective that it is making me think on issues I had not previously considered. But there are pieces to the puzzle still missing and some expert comments are suspect.
As to other gurus/experts - I usually shy away from them when I see supplements or books for sale, and as yet I have never bought any supplements from such places. I do buy all the books since I would not know if they have anything useful to say otherwise. The trouble with books is that they don't change easily when new science is revealed, and the authors usually feel committed to support what they have published even when new debates suggest they are wrong.
The only supplement I do take is magnesium since that prevents muscle cramps I have had for decades.
The PLAC Test is a blood test that measures an enzyme associated with the inflammation of your arteries. Having increased levels of Lp-PLA2 increase your risk of having a heart attack or stroke. In many adults, cholesterol causes a fatty deposit called plaque to build up in the walls of the arteries. Once arterial walls become inflamed, your body produces the enzyme Lp-PLA2. When the amount of Lp-PLA2 is high, this can indicate that the plaque is more likely to rupture through the inside lining of your artery into your bloodstream, where it may cause a clot that could result in heart attack or stroke.
Carbs are around 10-20g/day.
Fat is around 160g/day.
Expressed in terms of calories that would make fat around 78%, protein around 18%, and carbs around 4%.
And yes, I would be concerned with this amount of LDL-P.
"Excluding rare genetic mutations, why would a normal body create too much of a substance that will kill us?"
Because
people are eating bizarre diets liberal in butter and coconut oil
(which have been shown to down regulate the LDL receptor and raise serum
cholesterol), thinking that's what we are supposed to be eating. You
cannot compare hunter gatherers hunting down an antelope and eating its
brains and organs high in saturated fat and cholesterol to a modern
"paleo" eating bacon and eggs cooked in butter thinking they are doing
some kind of ancestral reenactment. Hunter gathers eat anything and
everything just to survive and reproduce, atherosclerosis in their 70's
is least of their worries. Not only that but they simply aren't not
eating 3 meals a day cooked in ghee, as the animal fats in the wild have
different fatty acid compositions . They are very active and probably
go through food shortages. Add in they also likely had cholesterol
lowering parasites that co-evolved with them and you'll see it's strange
to compare them to modern humans living in the modern sanitized world.
I
use some coconut milk myself so I'm hardly "anti saturated fat", but I
do acknowledge that it carries it's risks so I hardly think it's
responsible that diet guru's telling people they should be liberally eating butter, especially when I see the types of lipids people report almost daily after people "going primal". message...
MOST of your triglycerides come from body fat (NEFA released in excess of needs).
http://carbsanity.blogspot.com/2011/05/where-do-triglycerides-come-from-part-i.html
Unless you're a Type 1 or Type 2 diabetic this diet - IMHO - is insane long term.
mortality nearly doubled at either A1c 10.5% or A1c 6.0% compared with
A1c 7.5%"
Diabetics are at a disadvantage compared to non-diabetics because they have worse control over their BG level. I used a "driving down a road cut into the side of a mountain" metaphor to explain why maintaining higher mean BG level (which results in higher HbA1c) is preferable for diabetics on a high-GL diet. See http://nigeepoo.blogspot.co.uk/2010/02/problem-with-diabetes.html
As Evelyn says, non-diabetics have lowest mortality at HbA1c of ~5%.
Too much omega-6 fat concentrates fat & cholesterol in the liver (which lowers serum cholesterol).
Lack of choline also results in reduced fat & chol clearance from the liver.
Further down from this totem pole's top are primate studies, then various animal studies, and much further below are
Almost all your comments on this post have been hand-waving "makes sense to me" or "sounds good to me" type of "reasoning".
IMHO None of it rises to any level on which to base health behaviours
What importance do you place on small LDL-P?
Dr McDougall interviews Dr Atkins: High Carb vs Low Carb
Dr. William Davis
said...
Hi, Bix--
If there's one blunder I see in people who follow Atkin's-type diets is that they are exposed to excessive quantities of oxidized lipids or the poorly-named "advanced glycation end-products." Cooking with butter, heating meat at high temperature, and consuming
cured meats, while low-carb, has adverse effects.
Also, it wouldbe interesting to know the Apo E genotypes of these two men. I'll bet, for instance, that Nathan Pritikin was an Apo E4 kind of guy, making him more responsive to cutting fat in diet.
Keep up your great work.
February 3, 2011 at 3:59 PM
Design, Setting, and Participants
A controlled 3-way crossover design involving 21 overweight and obese young adults conducted at Children's Hospital Boston and Brigham and Women's Hospital, Boston, Massachusetts, between June 16, 2006, and June 21, 2010, with recruitment by newspaper advertisements and postings.
Intervention
After achieving 10% to 15% weight loss while consuming a run-in diet, participants consumed an isocaloric low-fat diet (60% of energy from carbohydrate, 20% from fat, 20% from protein; high glycemic load), low–glycemic index diet (40% from carbohydrate, 40% from fat, and 20% from protein; moderate glycemic load), and very low-carbohydrate diet (10% from carbohydrate, 60% from fat, and 30% from protein; low glycemic load) in random order, each for 4 weeks.
Although the very low-carbohydrate diet produced the greatest improvements in most metabolic syndrome components examined herein, we identified 2 potentially deleterious effects of this diet. Twenty-four hour urinary cortisol excretion, a hormonal measure of stress, was highest with the very low-carbohydrate diet.
Consistent with this finding, Stimson et al reported increased whole-body regeneration of cortisol by 11β-HSD1 and reduced inactivation of cortisol by 5α- and 5β-reductases over 4 weeks on a very low- vs moderate-carbohydrate diet. Higher cortisol levels may promote adiposity, insulin resistance, and cardiovascular disease, as observed in epidemiological studies. In a 6-year prospective, population-based study of older adults in Italy, individuals in the highest vs lowest tertile of 24-hour cortisol excretion, with or without preexisting cardiovascular disease, had a 5-fold increased risk of cardiovascular mortality.
C-reactive protein also tended to be higher with the very low-carbohydrate diet in our study, consistent with the findings of Rankin and Turpyn. Other studies also have found reductions in measures of chronic inflammation, including CRP with a low–glycemic index diet.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2968721/
Conclusions: High cortisol levels strongly predict cardiovascular death among persons both with and without preexisting cardiovascular disease. The specific link with cardiovascular mortality, and not other causes of mortality, suggests that high cortisol levels might be particularly damaging to the cardiovascular system.
While this isn't an absolute rule, one can find that even the sloppiest of published pieces and products maintain a generally 'okay' rating because of of ulterior-motive-driven support they receive from other parties in what soon becomes a network. To a random prospective customer who isn't aware of such a network, these disingenuous reviews become deal makers. So much for the integrity of the peer-review process.
http://www.livinlowcarbdiscussion.com/showthread.php?tid=10292
My last one done in 2009 showed NO calcium deposits in my arteries. I went back today, March 14, 2013, to have another one done to see what that 80-85% fat diet I've been eating is doing to me. My heart calcium score: ZERO
http://livinlavidalowcarb.com/blog/jimmy-moores-cholesterol-test-results-2008-2013/18256
and his last posted blood work shows a LDL-P of >2730
"i do not have any other radiology/lab data"
Here is Jimmy Moore's last COMPLETE blold work
http://livinlavidalowcarb.com/blog/jimmy-moores-n1-experiments-nutritional-ketosis-day-211-240/17390
Question - should he be concerned
Question - Can you go into a little more detail why you disagree with Dr Dayspring with regard to LDL-P and small LDL-P. It would be greatly appreciated.
Seriously, WTH ...
even when I was on very low fat in the late 80s McD rubbed me the wrong way.
In fact, lung dissection showed very heavy lung disease similar to coal-miner's lung disease (pneumoconiosis), and thus it is possible that inflammation was the cause of their atherosclerosis.
It is also sheer speculation to say that if you fed them bread, they would be certain to have MIs. Has this experiment been done? I do not think so....
My opinion is that the Inuit were exceptionally well adapted to the local environment and food. Let's not forget that these people walked across the Bering Strait from Siberia some 100,000 years ago. We know genetic selection effects can occur within a couple of generations. Just like the kitivar islanders, who are genetically adapted to their high carb diet, the ecological comparisons between cultures will only take you so far....they don't really tell us what we should be eating here in the west, where coronary disease is so common.
Maintain a healthy body weight and be moderate in your food choices. Going to any extreme (very high carb load or very high saturated fat load) will produce adverse consequences especially in vulnerable people (like me - a cholesterol hyperabsorber or someone very sensitive to saturated fat). I now consume a moderate fat vegetarian diet - mainly for ethical reasons, a tiny bit for health. MIs are multifactorial and diet is only one component of the problem.
with regard to LDL-P and small LDL-P. It would be greatly appreciated.
local environment and food."
There is no scientific evidence whatsoever to back up this claim.
"Let's not forget that these people walked
across the Bering Strait from Siberia some 100,000 years ago."
Inuits arrived in North America as as recently as ONE THOUSAND years ago.
"We know genetic selection effects can occur within a couple of generations."
Major changes in digestive anatomy and physiology take MILLIONs of years. Human have very few adaptations to modern diets such as an increased ability to digest starches and lactase persistence.The human digestive anatomy, physiology and gut flora is barely different from that of chimpanzees and bonobos.
"Just like the kitivar islanders, who are genetically adapted to their high
carb diet"
There is NO evidence that the Kitivans have any specific genetic adaptations to a high carbohydrate diet.
"the ecological comparisons between cultures will only take
you so far....they don't really tell us what we should be eating here in
the west, where coronary disease is so common."
The scientific community has known for 50 years that EVERYBODY should be eating a low fat (<10%), low protein (<15%) diet
based mostly on minimally processed whole plant foods. Anyone who claims otherwise is either ignorant or a charlatan.
http://www.carbsmart.com/5-health-markers-that-matter-more-than-total-cholesterol-and-ldl-c.html
3. LDL-P: LDL Particle number
There’s still some debate amongst the cholesterol experts about whether it is the total number of particles or the size of the particles that matters most. Since the science isn’t settled on this, we present both sides of that argument in Cholesterol Clarity and let the reader decide for themselves which side they choose to believe.
4. Small LDL-P: Small LDL Particle number
The Small LDL-P begins to become much more problematic when this number comprises more than 20 percent of your total LDL particles. For example, if your LDL-P is 1000, then your Small LDL-P needs to be 200 or less. Not to sound like a broken record, but if you consume less carbohydrates to your own personal tolerance level, and eat more healthy
saturated and monounsaturated fats in your diet, then your Small LDL-P will go down.
His small LDL-P percentage has gone UP from 6.4% to 17.5% between 10/12 and 4/13.
"I remember having my cholesterol tested with a standard lipid panel in early 2005, after losing 180 pounds the year before. My regular family doctor was out of the office on the day I went in to get the results and his analysis of my numbers. After looking at my test results, the fresh-out-of-school physician’s assistant filling in for him gazed up at me with a disturbing look of consternation. My total cholesterol was (to him) a shockingly high 225, and my LDL reading was a ghastly 130. He was adamant that I needed to be on a high-dose statin drug pronto. When I inquired about the stellar ratio between my HDL cholesterol (72) and my triglycerides (43), he admitted that those numbers were certainly in the good range, but quickly dismissed them as irrelevant to heart health. Keep in mind that I had just come off statin medications in 2004, and I had brought my weight down from 410 pounds to 230 pounds and was therefore getting healthier. He acknowledged that my triple-digit weight loss was impressive, but still wrote me a prescription for 40 mg of the cholesterol-lowering statin drug Lipitor."
Moore, Jimmy; Westman, Eric C. (2013-08-25). Cholesterol Clarity: What The HDL Is Wrong With My Numbers? (Kindle Locations 1756-1763). Victory Belt Publishing. Kindle Edition.
This would be a separate test, earlier, than the late October 2005 "normal" test. According to his blog he didn't even quit the statins until August 2005. Which story is true Jimmy? In his podcast with Diane Sanfilippo he said the LDL was 185 and TC 285 but the same HDL and trigs. Was that YET another test or just inflating things aka making up sheet aka lying?
The truth is Jimmy's diet is causing his abnormal lipids and from the looks of things it's not even working for the other stuff much any more.
Before I started on the Atkins diet in January 2004, I was told by my
family doctor to take statin drugs to control my cholesterol. First it
was Lipitor which just about killed my joints and muscles to the point
that I couldn't take the pain anymore. I pleaded with my doc to give me
something else to "lower my cholesterol," so then he switched me to
Crestor stating it wouldn't hurt me as bad. Boy was he wrong...it was
WORSE! A LOT worse!
In fact, I remember playing basketball at my church one night after losing 100 pounds in early 2004 while still taking Crestor when I went up for a rebound and felt the worst pain I've ever experienced in my thumb. I quickly ran to the sideline and saw my hand swelling up fast (I went to the emergency room where they said I had a deep tissue bruise). All I did was grab the basketball, but the joints in my fingers had become so weak that the impact of gripping the ball caused me to suffer an injury when it probably would not have happened had I not been taking a statin drug.
http://livinlavidalocarb.blogspot.com/2005/10/dum-da-dum-dum-my-blood-work-is-in.html
Tuesday, October 18, 2005
http://static.flickr.com/29/53696613_6a81cfebf3.jpg?v=0
TC - 201
Trigs - 57
HDL - 71
LDL - 119
SO - what happened between 10/05 and now???
http://livinlavidalowcarb.com/blog/my-cholesterol-craziness-continues/908
Check out the comparison of the numbers from March 2006 to April 2006:
LDL – from 172 to 230
HDL – from 72 to 57
Triglycerides – from 43 to 84
Total cholesterol – from 252 to 304
That’s when he said I probably have a genetic predisposition for
cholesterol issues which will need to be treated with several drugs
since my body can’t handle statins.
To that end, he prescribed for me to take the three following medications: Zetia, WellChol, and the prescription form of Niacin. My doctor said each of these have little to no side effects at all and will each lower the LDL by 10-15 percent. I relented and said I’d be willing to take these drugs if they won’t harm my body and will lower my LDL cholesterol.
Now I am taking these medicines because frankly I am concerned about the LDL continuing to rise.
My numbers, I think, are a lot like Cris: conventional markers (total cholesterol, HDL-C, LDL-C, triglycerides) all are classified as optimum, but LDL-p is elevated (1360) and small LDL is high (700). They didn't measure CRP, but Lp-PLA2 was low, in the optimum range (suggesting low inflammation). The LP-IR score places me at the midpoint of the insulin sensitivity/resistance spectrum. I was previously prediabetic based on A1C, am now high normal (5.5-5.7), so some degree if IR is not surprising.
I had been following a relatively low carb diet, and lost some weight. Have since regained about half of the weight that I had lost, and am presently eating a moderate level of carbs (at least 100 per day, probably more). So what shall I do? Unlike Cris, I have room to reduce my carb intake. So I'm thinking dial back the carbs, but stay away from NK, try to lose some weight, and... ??? (I'm already on a low dose statin, would be reluctant to push the dose up, and don't want to add niacin to the regime.)
Looking at Jimmy's cholesterol history, it doesn't look like he ever had a satisfactory LDL-p. His conventional markers looked better at points in the past, but there is no LDL-p associated with that, so we don't know if going back to that old way of eating and exercising would really get him out of the danger zone. I assume the advice from this group would be to try what worked better before. But if his LDL-p was still high, then what?
"only one solution for all"
I've had the perception the last couple of years that he doesn't even hear some questions that he gets asked. For a polititian to answer the question he wants to instead of what's asked is fine but for health advocates ...
Cherry picking confirmatory studies and ignoring dis-confirmations (SOP or par for the course in the diet field)
I don't know your age or media exposure but for me the salient comparison's between Covert Bailey & McDougall. There were a lot of others of course, I've forgotten many - Francis Lappe is another that just occurred to me. My perception even comparing him to his 80s low fat colleagues (I was a die hard low fatter in the late 80s) is of a total sourpuss and inflexible absolutist.
[0] the major caveat being I have not gone through his entire corpus. I left doctrinal, dogmatic low fat behind a long time ago even though these days I occasionally end up doing very low fat for a week at a time - all I had last week was tuna, chicken breast, yogurt (made myself with fat free skim milk), potato, apples, cantaloupe and 500g liver.
things might be different if his audience hadn't selected out critics ...
I consulted with a nephrologist and haematologist. The nephrologist thought out loud about wanting to put me on statins.
(!!!!!!!!) (???????)que? [0] (!!!!!!!!!!!)
Not one of my cholesterol tests had ever approached the high end.
I've asked around and did some googling but still canNOT for the life of me figure out why a nephrologist would even think about that.
The haematologist just smiled & shook his head, offered no comment when I (I think tactfully) asked why a nephrologist might float the idea.
so yeah ... doctors believing cr*p ... what's hard to believe is why you find it hard to believe
[0] wtf does not describe by reaction well enough
You probably know which foods are rich in cholesterol and saturated fat. What people often don't know is which legumes, fruits, vegetables, grains, nuts, seeds etc are "safe" to consume from a carb standpoint. For example, white chickpeas are very high in starch, but black chickpeas are very low in starch (and higher in protein, I might add). It took some experimentation to figure out how to add some grain back to my diet - essentially I use wheat bran, wheat germ and hemp protein powder (and nothing more). This limits carb intake dramatically. Re: fruit, I stay away from everything except tomatoes and avocados. However, half a kiwi fruit is only about 4 g of net carbs - not bad, but I would rather do without. Again, the tightrope.
I also had insulin resistance and hypercholesterolemia - this is a double whammy, and the treatment through diet means restricting saturated fat, cholesterol and free carbs. There are additional ways to get LDL down such as consuming more almonds, soy, fiber, and omega-6's (god forbid!).
DIET AND SEBUM CHOLESTEEOL IN MAN: LACK OF EFFECT OF DIETARY CHOLESTEROL
ANCEL KEYS, J. T. ANDERSON, OLAF MICKELSEN, SADYE F. ADELSON AND FLAMINIO FIDANZA
Outcome:
Cross-sectional surveys in Minnesota on young men - no relationship between dietary cholesterol and the total serum cholesterol concentration
Two surveys on Island of Sardinia - failed to show any difference in the serum cholesterol concentrations of men of the same age, physical activity, relative body weight, and dietary pattern, but differing markedly in cholesterol intake
Carefulstudy during 4 years with 33 men whose diets consistently very low in cholesterol - serum cholesterol values did not differ from 35 men on very high cholesterol diet
Comparisons made of 23 men before and after they doubled their cholesterol intake and of 41 men who halved their intake - failed to show any response in serum cholesterol level in 4-12 months
Detailed study of the complete dietary intakes of 119 Minnesota businessman - failed to show any significant increase in serum cholesterol with increasing dietary cholesterol intake
4 completely controlled experiments on men - addition or removal of 500-600mg of cholesterol a day had no effect on serum cholesterol
Completely controlled experiment on 5 physically active men -
changing from a diet of 500 mg cholesterol to 0 mg of cholesterol had no effect on serum cholesterol
In completely controlled experiment in 13 men - no significant effect in changing cholesterol from 374 mg/day to 1369 mg/day, or from 1369mg/day to 374 mg/day on serum cholesterol.
Comments:
The foregoing evidence is definitive, we think, in showing that variations in the intake of cholesterol over the whole range of natural diets do not influence the serum level of physically normal adult men so long as other elements in the diet are constant.
They conclude that “in adult men, the serum cholesterol is essentially independent of the cholesterol intake.”
NOW - show me definitive proof that a low fat, low protein diet is a diet that EVERYONE should follow.
If high lipid values can cause damage then test to see if actual damage has occurred or is occurring. If those tests show little to zero abnormalities then those high lipid values have little if any meaningful value. So test calcium scores, hsCrp, etc, and if they show no issues then forget the lipid results. That was the message I took from the book, and most of the practicing MDs seemed to support that.
I also note that the current lipid/statin dogma was generated based on high carb diets, and or high carb and high fat. That means that insulin will be present at levels that consistently inhibit lipolysis and hence prevent sustained ketosis. In a fat adapted ketogenic state the metabolism is significantly different than that based on primarily glucose. When burning primarily fat and generating high rates of ketones then a very different rate of lipid traffic and usage is active. It is very unclear what the lipid numbers mean in a ketogenic state especially when all other health markers look exceptionally good.
I am not particularly interested in supporting Jimmy or criticizing him. That activity seems to distract from the more interesting actual issues. Almost all books in the diet/health/nutrition arena appear biased or misleading in some ways, but those of us who read a lot and can see the bigger picture can usually see past those discrepancies and move on. Let's take what we can. Or in other words are we primarily book critics here or are we more interested in the issues raised by the book?
As to Jimmy, I would cross that bridge when I got to it. If his LDL-P is still high on LCHF but not the uber buttery sort, "low" weight and regular exercise, then maybe the diet should still be reconsidered. He has not embraced olive oil ....
Unfortunately there is almost ZERO fact checking in the popular press and pretty much anyone can claim anything with no accountability if anyone follows their advice. There's a woman Jimmy had on his LLVLC podcast with a book out on a keto diet for cancer. It turns out she had conventional chemo, hasn't even had a full follow up, is only a few years post-remission, etc. ... but still credits her diet. That is supremely irresponsible ... but disclaimers let it go.
guess that for image reasons, real pharmaceutical companies would prefer
to avoid agents that have been sold previously with questionable claims by the health food indsutry.
> easily avoided by taking CoQ-10
I've been working under the impression that oral Co-Q doesn't survive digestion in significant amounts ...
The Effect of High-, Moderate-, and Low-Fat Diets on Weight Loss and Cardiovascular Disease Risk Factors
One hundred men and women followed one of four dietary programs for 1 year: a moderate-fat (MF) program without calorie restriction (28 patients); a low-fat (LF) diet (phase I) (16 patients); a MF, calorie-controlled (phase II) diet (38 patients); and a high-fat (HF) diet (38 subjects). Weight, total cholesterol (TC), low-density lipoprotein cholesterol
(LDL-C), high-density lipoprotein cholesterol (HDL-C), triglycerides (TG), homocysteine (Ho), and lipoprotein(a) [Lp(a)], were measured every 4th month. The TC/HDL-C ratio was calculated and fibrinogen levels were measured at baseline and after one year.
Only patients following HF diets showed a worsening of each cardiovascular disease risk factor (LDL-C, TG, TC, HDL-C, TC/HDL ratio, Ho, Lp(a), and fibrinogen), despite achieving statistically significant weight loss.
Dietary Regimens
High-Fat (HF) Diet This diet is defined as one in which patients consume 55%-65% of their daily caloric intake in the form of fat calories. Less than 100 g of carbohydrates (RCHO) were consumed daily and protein intake constituted 25%-30% of the total caloric intake. Patients ate until satiated.
Moderate-Fat (MF) Diet Patients following this dietary program consumed 20%-30% of their calories in the form of fat. Approximately 60% of their calories were from carbohydrate sources and the remaining calories were derived from protein. Patients consumed 10–12 calories per pound per day on this diet.
MF, Calorie-Controlled (Phase II) Diet Patients following this program were asked to consume 350–500 fewer kilocalories per day than required to maintain body weight. This was determined by multiplying their current weight in pounds by 10 kcal/lb to determine
the required kcal intake per day; 350–500 was subtracted from this figure to determine the desired daily intake of calories. Of these calories, 15% were protein and 70% were carbohydrate, with an emphasis on complex carbohydrates vs. simple sugars. The remaining 15% of the calories could be consumed as fat in a 2:1 ratio of nonsaturated
(polyunsaturated and monosaturated) to saturated fat, with no more than 5g of saturated fat intake per day.
Low-Fat (LF) (Phase I) Diet The LF diet consisted of fruits, vegetables,a limited amount of grain/cereals for breakfast and a multiple vitamin that included 100% of the US Department of Agriculture recommended daily intake of vitamins and minerals. Patients ate until satiated. Of the caloric intake, 10% was fat, 15% was protein, and 75% was carbohydrate, with an emphasis on complex vs. simple carbohydrates as shown in Table
I.
SO - WWJS (What Would Jimmy Say)
A year or two ago, when I was trying harder to be low carb, I ate more cheese, ham, red meat, sausage, etc. then I do now. But I never fully bought into the idea that high saturated fat was benign, or desirable, and eventually shifted toward the fats that are more traditionally considered healthy.
These days, I'd describe my eating as higher carb south beach, or lower carb Mediterranean I eat eggs for breakfast, use half and half in coffee. Rarely eat cheese, use 1% milk, use lots of olive oil for cooking, lots of salads with olive oil dressing, snack on almonds. Animal protein is typically from chicken or fish, with beef occasionally, usually a leaner cut. About the only processed foods I eat are Kashi or Southbeach granola bars (for the convenience). The latter do have some saturated fat; the former are mosly almond sources of oil. Also take fish oil supplements, for a goodly amount of omega 3's.
So I don't think I would be super high on saturated fat, and not over the top in terms of overall fat consumption. I had been cutting back fat somewhat (and increasing carbs - more fruit, modest amounts of beans, rice and potatoes) as I tried to rein in calories.
As I've gone up in carbs, my triglycerides have risen, for the 50-70 range up to the 100-120 range. LDL, HDL, and TC haven't changed much, still 'excellent' by conventional standards.
Could probably cut both carbs and saturated fat, but not drastically.
I just found this
The Role of Coenzyme Q10 in Statin-Associated Myopathy
SO ... not so cut and dried and established as I remembered so I semi-retract my comment but I'll leave it there. Personally I have known a few people for whom CoQ helped. Placebo? Don't know. At the end of this 2007 review:
Statin therapy is frequently limited by myopathic symptoms creating a critical need for strategies to prevent statin myopathy. Coenzyme Q10 supplementation is a simple, attractive therapy that requires an appropriately powered and randomized trial to determine whether CoQ10 eliminates or reduces statin myalgia in symptomatic patients. Simultaneous genetic studies should attempt to determine if genetic variants contribute to the variability in the response to CoQ10 therapy. Studies designed to determine if CoQ10 prevents the onset of myalgia in statin-naive patients are not practical because of the number of subjects that would be required in such a trial. In addition, the absence of pharmacologic grade CoQ10 supplement and a study sponsor makes such a trial difficult. Nevertheless, such trials are the only way to demonstrate conclusively whether or not clinicians should prescribe CoQ10 to their patients on statin therapy.
To me this at least falls into the if you experience the symptoms, it probably can't hurt to try the CoQ.
- 10% fat of what? A 200 calorie diet or at. . . oh, I'm repeating myself.
- Definitive proof doesn't exist for anything, but more recent modern populations have done fine on low fat and better than other groups. Okinawans from not that long ago say 'hai'. Most cultures use fat for flavouring and it helps with vitamin absorption. This doesn't mean that food has to be swimming in fat and plenty of natural sources of mineral rich foods do contain fat. Have a look at daily EFA requirements, which clock in at about 30 or so grams. Hell, add in a few more grams of fat from butter or dairy or whatever. You're still looking at 10-15% fat in the context of a 2500 calorie diet.
Calories have to come from somewhere. Show us definitive proof that when calories come primarily from carbohydrate, with fat simply serving as a small granish (yes, usually in the 10% mark of a total, non-hypocaloric diet), that individual subjects suffer poor health, inflammation and glycate to hell. Again, many long-lived populations stand in the way of the false dichotomy that is created from these definitive arguments.
And some people do absorb dietary cholesterol, including the oxidised variety.
Post a Comment
Comment Moderation is ON ... I will NOT be routinely reviewing or publishing comments at this time..